Seven years after the Food Allergen Labeling and Consumer Protection Act[1] (FALCPA) went into effect, unlabeled allergens continue to be the leading cause of recalls and a leading cause of reportable foods for U.S. Food and Drug Administration (FDA)-regulated foods. The presence of unlabeled allergens presents a significant health hazard for food-allergic consumers, and allergen recalls represent an economic burden for industry and a resource need for FDA.
Allergic consumers rely on food labels to be complete, clear and accurate so that they can avoid exposure to foods or ingredients that can provoke potentially life-threatening reactions. This is particularly important because data from the U.S. Centers for Disease Control and Prevention (CDC) show that the number of food-allergic consumers is increasing as are the number of hospital visits related to food allergies and allergic reactions.2 To help food-allergic consumers find and understand the information they need, FALCPA designated those food allergens of greatest public health concern in the U.S. as the major food allergens (milk, egg, peanut, soy, fish, crustacean shellfish, wheat and tree nuts), described the two formats that can be used to declare the presence of major food allergens and required the use of the common or usual name of the food source for the major food allergens (e.g., declaring milk when casein is used as an ingredient). FALCPA also requires the declaration of major food allergens that are components of flavorings, colorings and incidental additives.
Before FDA and the food industry can develop practical approaches to reducing the number of food allergen recalls, it is important to understand the nature of the problems that lead to these recalls, the foods that are most often affected and the allergens that are most often involved. For FDA-regulated products, this information can be found in the FDA Reportable Food Registry (RFR) and the FDA Recall Enterprise System (RES) databases (see “What Is the Reportable Food Registry?”). A close look at the allergen-related entries in these databases shows that there are clear patterns and trends, and suggests that the number of food allergen recalls can be significantly reduced through improved awareness and simple changes in the way that packages, labels and ingredients are handled and tracked within production facilities.
Reportable Foods and Allergen-Related Recalls: The Numbers
 The RFR collects mandatory reports from industry and voluntary reports from public health officials related to foods that represent serious health risks. These risks include the presence of undeclared allergens, microbial pathogens, foreign objects and other hazards. Over the RFR’s first 3 years (September 2009 to September 2012), about 90 percent of all reports involved three hazards: Salmonella, Listeria monocytogenes and undeclared allergens, with undeclared allergens accounting for essentially the same number of reports as Salmonella (34 percent and 36 percent of all reports, respectively) (Figure 1). During these 3 years, the proportion of reports for undeclared allergens increased from 30 percent of all reports in the first year to 40 percent of all reports in the third year.
The RFR collects mandatory reports from industry and voluntary reports from public health officials related to foods that represent serious health risks. These risks include the presence of undeclared allergens, microbial pathogens, foreign objects and other hazards. Over the RFR’s first 3 years (September 2009 to September 2012), about 90 percent of all reports involved three hazards: Salmonella, Listeria monocytogenes and undeclared allergens, with undeclared allergens accounting for essentially the same number of reports as Salmonella (34 percent and 36 percent of all reports, respectively) (Figure 1). During these 3 years, the proportion of reports for undeclared allergens increased from 30 percent of all reports in the first year to 40 percent of all reports in the third year.
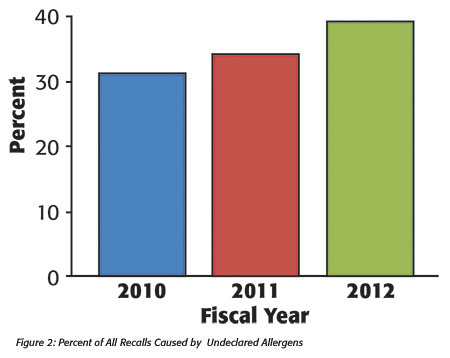 Reportable foods are foods that pose a risk of serious adverse health consequences or death to consumers. This standard is the same as that for FDA Class I recalls, so the number of primary RFR reports for unlabeled allergens is similar to the number of Class I allergen recalls. In addition to these recalls, there are a large number of Class II allergen-related recalls. Allergen recalls are considered to be Class II when the only allergen involved is wheat or when other mitigating circumstances reduce consumer risk. For example, a food label that declares the presence of one tree nut on a food that contains a different tree nut is typically considered to be a Class II hazard because most tree-nut-allergic consumers avoid all tree nut-containing products. In addition, labels that declare the presence of an allergen-containing ingredient (such as butter) without declaring the allergen (milk) by using the common name of the food are often classified as Class II recalls when the ingredient is commonly known to contain the allergen (see “FDA Recall Classification,”). Allergen recalls increased steadily over this 3-year period (Figure 2).
Reportable foods are foods that pose a risk of serious adverse health consequences or death to consumers. This standard is the same as that for FDA Class I recalls, so the number of primary RFR reports for unlabeled allergens is similar to the number of Class I allergen recalls. In addition to these recalls, there are a large number of Class II allergen-related recalls. Allergen recalls are considered to be Class II when the only allergen involved is wheat or when other mitigating circumstances reduce consumer risk. For example, a food label that declares the presence of one tree nut on a food that contains a different tree nut is typically considered to be a Class II hazard because most tree-nut-allergic consumers avoid all tree nut-containing products. In addition, labels that declare the presence of an allergen-containing ingredient (such as butter) without declaring the allergen (milk) by using the common name of the food are often classified as Class II recalls when the ingredient is commonly known to contain the allergen (see “FDA Recall Classification,”). Allergen recalls increased steadily over this 3-year period (Figure 2).
Food Allergen Recalls: Beyond the Numbers
To dig into the details behind the numbers and to better understand what problems were leading to these recalls, the information for each food allergen recall contained in the FDA RES database was reviewed. RES contains information on all recalls of FDA-regulated products entered by agency recall coordinators and field investigators. Each entry includes a description of the product(s) involved, the nature of the problem that led to the recall and may contain additional information on the root cause. The RES entry for each primary food allergen recall that occurred during the same 3-year period was examined to identify the food involved, the unlabeled allergen(s) and the root cause (when this information was available). The foods involved were classified using the same system used for the RFR database. (A detailed description of these commodity definitions can be found on the FDA web site.[3])
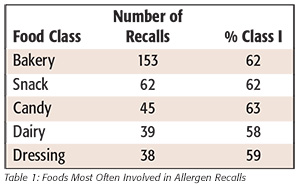 The five food types that were most often involved in food allergen recalls during this period were bakery products, snack foods, candy, dairy products and dressings (Table 1). Bakery products accounted for almost as many food allergen recalls as all of the other top five foods combined. The proportion of Class I recalls ranged from 63 percent for candy to 58% for dairy.
The five food types that were most often involved in food allergen recalls during this period were bakery products, snack foods, candy, dairy products and dressings (Table 1). Bakery products accounted for almost as many food allergen recalls as all of the other top five foods combined. The proportion of Class I recalls ranged from 63 percent for candy to 58% for dairy.
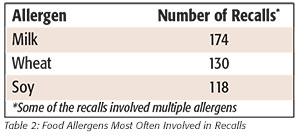 The allergens most often involved in recalls were milk, wheat and soy (Table 2). There were fewer recalls involving peanuts and tree nuts combined than for any of these top three allergens. Just over 20 percent of the recalls involved mislabeling for multiple allergens. Many of the recalls that involved more than one allergen combined milk, wheat, soy and egg. This may reflect the many different ways that these foods are used and the variety of different ingredients that are derived from each of them.
The allergens most often involved in recalls were milk, wheat and soy (Table 2). There were fewer recalls involving peanuts and tree nuts combined than for any of these top three allergens. Just over 20 percent of the recalls involved mislabeling for multiple allergens. Many of the recalls that involved more than one allergen combined milk, wheat, soy and egg. This may reflect the many different ways that these foods are used and the variety of different ingredients that are derived from each of them.
Only about 20 percent of the recalls for soy involved soy lecithin; however, it was not possible to tell whether these involved the use of lecithin as a release agent or as an emulsifier.
Because of the variety of foods involved in allergen recalls during this period, it was not possible to carry out a detailed analysis of the most common allergen/food combinations. However, information in the RFR database showed that within the bakery products category, cookies and cakes were the most often reported food types. Within the candy products category, a large number of reports were caused by the presence of undeclared milk in products containing dark chocolate. Among the snack foods, there were several recalls for chocolate-coated snack bar products that carried “dairy-free” or “vegan” labels. In many cases, these snack bar products were made on shared equipment that was also used to manufacture products with milk chocolate. The levels of milk found in some of the vegan products represented a significant risk for milk-allergic consumers, particularly if the consumer assumes these products are completely dairy-free.
Looking at Root Causes
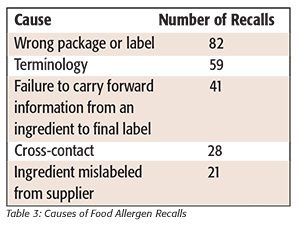 Understanding why food allergen recalls occur is critical for finding ways to reduce the number of these recalls and, therefore, the risk to allergic consumers. Root cause information was available in the RES database for about 67 percent of the allergen recalls. Overall, 13 distinct root causes were identified. Of these, use of the wrong package or the incorrect label for a product was the most common problem (Table 3). Although there were a variety of reasons why manufacturers used the wrong package or applied the incorrect label, one frequent problem was that packages for similar products made with different allergens, or products with and without allergens, looked very similar. In many cases, it was difficult for workers to distinguish packages or labels when they were handled in bulk. When packages look similar, it is easy for a worker to grab the wrong package or roll of film, especially in the middle of a production run. The use of similar-looking packages also makes it difficult to maintain accurate and detailed inventory records that might be used to recognize that mislabeling has occurred. Problems related to failure to remove unused packages or labels after a production run or during product changeover were also common.
Understanding why food allergen recalls occur is critical for finding ways to reduce the number of these recalls and, therefore, the risk to allergic consumers. Root cause information was available in the RES database for about 67 percent of the allergen recalls. Overall, 13 distinct root causes were identified. Of these, use of the wrong package or the incorrect label for a product was the most common problem (Table 3). Although there were a variety of reasons why manufacturers used the wrong package or applied the incorrect label, one frequent problem was that packages for similar products made with different allergens, or products with and without allergens, looked very similar. In many cases, it was difficult for workers to distinguish packages or labels when they were handled in bulk. When packages look similar, it is easy for a worker to grab the wrong package or roll of film, especially in the middle of a production run. The use of similar-looking packages also makes it difficult to maintain accurate and detailed inventory records that might be used to recognize that mislabeling has occurred. Problems related to failure to remove unused packages or labels after a production run or during product changeover were also common.
The second most frequent cause of allergen recalls was the use of the wrong terminology in the ingredient list or the allergen “contains” statement. For example, a product might declare the presence of butter but not milk, or the presence of tree nuts but not the specific type of nut or the presence of flour but not wheat. It is not clear why there are so many terminology problems or why the number of these recalls is not decreasing over time. About one-half of the recalls caused by this problem were for bakery products.
The third most common cause of allergen recalls was failure to carry forward allergen information from an ingredient to the final product label. In some cases, the failure to carry forward allergen information resulted from changes in an ingredient formulation by a supplier; in others, it was caused by changing ingredient suppliers to one with a different formulation. In other cases, allergen information was difficult to find on the ingredient labels, because it was not declared in a standard format or location on containers for bulk ingredients. Frequently, the certificate of analysis or product specification sheet for a bulk ingredient was sent to a customer separately from the actual lot of the ingredient, and the allergen information in these documents was not reconciled with the expected allergen content for the ingredient. These situations show that it is important for an ingredient user to develop procedures to recognize and respond to changes in ingredient formulations (see “RFR Notable Outcomes,”).
Emerging Issues Indicated Through RFR Reporting
Several trends seen in food allergen-related RFR reports may be signals of emerging issues that will become common in the next few years. One of these is an increase in labeling errors caused by the use of incorrect, outdated or damaged data files in computerized on-site label printing systems. The ability to print labels during manufacture or directly on packaging provides tremendous flexibility and cost savings for producers, but also creates new opportunities for errors and omissions unless controls are in place to ensure that the correct data or template files are used and that these files have not been corrupted. For example, several recalls have been caused by an employee clicking on an old (outdated and incorrect) version of a label file when loading data into a printer system. In several other cases, a label file generated at a central corporate location was used at a remote production site without checking to see if the ingredients actually being used matched those on the label.
Reports of problems related to allergen labeling of imported foods and ingredients are increasing. Within the RFR database, reports involving undeclared allergens increased from 13.2 percent of the reports for imported foods in year 1 to 19.6 percent of the reports for imported foods in year 3. Imported foods present some unique and difficult challenges, particularly when they involve a chain of suppliers. Foods or ingredients that contain major food allergens (as defined in the U.S.) might not need to be identified in the country (or countries) where they are produced or combined, leading to the presence of undeclared allergens in imported products. Problems like this are likely to become more common as the food production system grows more complex and more international over the coming years. A related problem stems from the increasing number of food products that are imported in consumer-ready packages. In some cases, these packages carry allergen declarations that are appropriate in the country of origin, or in other markets such as the European Union, but not in the U.S. One significant source of confusion is the different lists of allergens of public health concern in different countries. It is important to note that products for the U.S. market must meet U.S. requirements, including requirements about allergen declarations.
What Have We Learned from This?
The most important lesson learned from this analysis of food allergen recalls and reportable foods is that many of these recalls were caused by simple problems and could have been easily avoided. For example, the food industry could implement a regular review process to look for formulation changes in products and ingredients, which is not complicated or time-consuming but can provide insurance against unexpected serious problems. Similarly, double checks of packages and labels before they are used to ensure that they match the product being produced can be carried out in seconds and can avoid costly mistakes.
A second important lesson is that packing and label controls are as important for allergen control as are sanitation and Good Manufacturing Practices (GMPs). Allergic consumers rely on food labels to be accurate and complete. While GMPs and preventive controls are critical in averting the unintended presence of allergens through cross-contact, it is just as important to be sure that all the allergens that are used or that are components of ingredients are declared.
The third important lesson is that allergen-related problems occur more frequently in some types of foods than in others. In some cases, such as when using shared equipment to make different types of chocolate products, this reflects the difficult nature of the product. In other cases, such as the production of dry mixes, this reflects the nature of the production environment.
The final lesson is that ongoing monitoring of recalls and RFR reports provides important early warning signals that can be used to identify emerging issues and trends.[4]
Steven M. Gendel, Ph.D., is the FDA food allergen coordinator. He has extensive experience in food allergen control, food safety risk analysis, hazard evaluation and informatics. He has a B.Sc. in chemical engineering from Case Western Reserve University and a Ph.D. in cell and developmental biology from the University of California, Irvine.
Jianmei Zhu, Ph.D., is currently an ORISE fellow with FDA’s Center for Food Safety and Applied Nutrition. She works on risk analysis of food allergens. She received her Ph.D. in biochemistry and molecular biology from Johns Hopkins University in 2012 and her B.Sc. in biological science from Shanghai Jiao Tong University in China.
Nichole Nolan, M.P.H., is a program analyst in the Office of Analytics and Outreach with FDA’s Center for Food Safety and Applied Nutrition managing the RFR program. She graduated from University of Maryland, College Park with a B.Sc. in molecular biology and genetics and subsequently obtained her M.P.H. at Johns Hopkins University.
Kathy Gombas is a senior advisor in the Office of Compliance with FDA’s Center for Food Safety and Applied Nutrition. She is the co-lead for FDA’s Food Safety Modernization Act Implementation Change Management effort. Kathy received her B.Sc. in microbiology from Northern Arizona University. She is on the Editorial Advisory Board of Food Safety Magazine.
References
1. www.fda.gov/Food/GuidanceRegulation/GuidanceDocumentsRegulatoryInformation/Allergens/default.htm.
2. www.cdc.gov/nchs/data/databriefs/db10.htm and www.cdc.gov/nchs/data/databriefs/db121.htm.
3. www.fda.gov/downloads/Food/ComplianceEnforcement/UCM211534.pdf.
4. Gendel, S.M. and J. Zhu. 2013. Analysis of U.S. Food and Drug Administration food allergen recalls after implementation of the Food Allergen Labeling and Consumer Protection Act. J Food Prot 76(11):1933–1938.
p>




