There is a treasure trove of handwashing science lying dormant, awaiting implementation. Year after year the bank of scientific knowledge grows yet foodborne illness risks associated with poor handwashing in the food industry persist. Science and technology are on an obvious path of continuous improvement but handwashing frequency—and therefore, adequacy as a food safety measure—is not. Unfortunately, the assets that handwashing science offers us remains largely frozen, yielding an unnecessarily high level of risk to the food industry and to its customers.
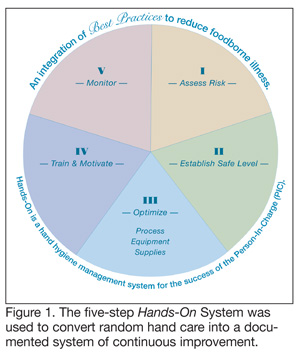 The Handwashing for Life Institute, an international organization devoted to advancing the science of hand hygiene with the purpose of reducing the incidence of foodborne illness caused by poor hand hygiene, set out to utilize today’s technologies in an integrated system of best practices. This body of knowledge, simply titled Hands-On, has been engineered to significantly reduce the risk of foodborne outbreaks by improving hand hygiene behaviors through a five-step system. These five steps—assessing risk, establishing safe levels, optimizing processes, equipment and supplies, training and motivating personnel, and monitoring—weave the science with the arts of management and food handler motivation (Figure 1). Essentially, the Hands-On five-step system deploys the science and technology we possess to help us achieve the behaviors we seek—namely, best-practice-level handwashing protocols and practices that translate into the pay-off of greater handwashing compliance and improved food safety throughout the food supply chain.
The Handwashing for Life Institute, an international organization devoted to advancing the science of hand hygiene with the purpose of reducing the incidence of foodborne illness caused by poor hand hygiene, set out to utilize today’s technologies in an integrated system of best practices. This body of knowledge, simply titled Hands-On, has been engineered to significantly reduce the risk of foodborne outbreaks by improving hand hygiene behaviors through a five-step system. These five steps—assessing risk, establishing safe levels, optimizing processes, equipment and supplies, training and motivating personnel, and monitoring—weave the science with the arts of management and food handler motivation (Figure 1). Essentially, the Hands-On five-step system deploys the science and technology we possess to help us achieve the behaviors we seek—namely, best-practice-level handwashing protocols and practices that translate into the pay-off of greater handwashing compliance and improved food safety throughout the food supply chain.
Step 1: Assess Risk
An assessment of risk in the context of rising brand values, business continuity and annual growth goals is a good exercise for food company senior executives. While there are some missing links in the science—i.e., some “nice-to-haves”—the principle gap in establishing good handwashing compliance in food processing, foodservice and retail operations is that the “must have” commitment is nowhere near the food labs and test kitchens. It is in the boardroom. Breaking this boardroom barrier is priority one and the focus of Step 1 in the proposed Hands-On solution.
Almost all food company mission statements acknowledge the importance of food safety, often under a general headline of “quality.” Once written, there is an assumption that a department or more likely, multiple departments, will apply this factor as they leverage their particular professional skills in adding value to the company’s products and brands while reducing costs. The reassuring “in control” language of mission statements and annual reports can mask the growing gap between actual current practices and needed safe levels of handwashing.
This compliance gap is rooted in the tendency to trivialize the importance of handwashing compared to more measurable investments, such as a new convection oven system that reduces cooking times by “x”, costs by “y” and raises profits by “z.” The board feeds on corporate math, and in particular, on measurable return-on-investment (ROI). We all know that what gets measured gets budgeted first. But where are the measurements of risk for operating at perhaps half-safe handwashing levels? Where are any measurements related to handwashing? Without numbers the topic is easily trivialized and left as a game of chance.
Foodborne illness outbreak risk is, and forever will be, synonymous with serving food to the public. Handwashing is just one more factor to manage but one that must be addressed more aggressively—sufficient to match up with the aggressive lawyers armed with DNA technology and poised to defend any one of your customers. The threat is much greater than the workman’s comp, slip/fall or chipped teeth cases that have dominated the agendas of many risk management departments.
After very successful rounds of investment in temperature control, handwashing is now the biggest single remaining threat to serving safe food. Controlling equipment has proven to be considerably easier than controlling handwashing behaviors. Motivation, training and employee turnover become factors. We must now learn to control a process that has never been under control. And let’s face it, ignoring handwashing as a priority is easy until a company is faced with a crippling outbreak of foodborne illness. It is often summarized in the feeling that there is nothing that can be done, or “We’re doing all we can.” Some will correctly say the real problem is keeping ill employees out of the kitchen and keeping ill customers at home (i.e., cruise ship passengers).
An understanding of the legal principle of strict liability will quickly change that attitude for all but the high-roller risk-taker. This intangible handwashing factor with its lack of standards must be met head-on with the same rigor and level of professionalism as major menu changes. As food safety professionals, we must not let the board be discouraged by these three realities: 1) the risk will never be zero; 2) the risk is rising in spite of the food getting safer; and 3) ill employees and ill customers are a constant threat to the health of your business. The universal precaution is handwashing.
Publicized losses due to foodborne outbreaks generally focus on the legal settlements. This dollar value is dwarfed by the unstated losses in sales and lost opportunity. Last year, a foodservice chain endured what was described by attorneys with Seattle, WA-based Marler-Clark as the “largest payout ever awarded” to their long list of clients over their 10-plus years of specializing in foodborne outbreak litigation. Along with the legal judgment came a significant drop in stock value and a painful 10 months that saw the restaurant manager released along with his area manager. Eighty jobs were lost because the restaurant was unable to recover. The building remains vacant.
Ultimately, risk is operationally specific and directly linked to the people served, the people handling the food, the menu, the facility and the level of process control or hand hygiene practices and training. Because these factors vary considerably from operation to operation, a self-assessment by each operator to identify the areas of potential or existing risks is recommended. Again, the total risk for foodborne illness can never be eliminated but it can be managed. A good approach is to institute an executive review of the total potential impact of foodborne illness related to poor handwashing that is passed along to multifunctional groups in the organization to engender an integrated response. Operational plans should be headed up on a day-to-day, shift-to-shift basis by the person-in-charge (PIC), who will be directly responsible for any foodborne illness contracted by the customers or their fellow employees as a result of eating, visiting and/or working at their establishment. A multi-disciplined assessment of risk factors should be carried forward to the next step in the program: setting safe levels for the quality and frequency of handwashing, hand sanitizing and gloving. In this way, operators will be able to pinpoint the highest level areas of concern and reduce the incidence of poor handwashing practices.
Step 2: Establish Site-Specific Safe Levels
 Establishing and monitoring a standard for the quality of the handwash is a must. Graphic tools are recommended wherever possible, as these become important training aids. First, conduct a self-assessment of skin condition, using this as an opportunity to demonstrate that healthy skin is easier to wash and that dry, cracked skin requires additional attention. Second, deploy a germ simulation using a tracer such as GlitterBug. Coat the hands of a trial group, wash according to your average practice. Illuminate individually with an ultraviolet (UV) light and transfer your findings to a ProGrade (or similar) form (Figure 2). By marking these hand outlines you can now develop a scoring system and set a “safe level” of handwashing quality as a minimum standard.
Establishing and monitoring a standard for the quality of the handwash is a must. Graphic tools are recommended wherever possible, as these become important training aids. First, conduct a self-assessment of skin condition, using this as an opportunity to demonstrate that healthy skin is easier to wash and that dry, cracked skin requires additional attention. Second, deploy a germ simulation using a tracer such as GlitterBug. Coat the hands of a trial group, wash according to your average practice. Illuminate individually with an ultraviolet (UV) light and transfer your findings to a ProGrade (or similar) form (Figure 2). By marking these hand outlines you can now develop a scoring system and set a “safe level” of handwashing quality as a minimum standard.
This graphic self-learning system helps convey important procedures in a memorable way with very few words. Employees will see for themselves why the traditional “splash ‘n dash” method is ineffective while gaining a visual understanding of the company’s fingernail and jewelry policies as part of the overall personal hygiene program. A further specification for hand cleanliness can be set and monitored using bioluminescence technology.
In establishing safe levels, employee exposure to the Hepatitus A virus should be taken into account. Is this virus present in the local community or in those places visited by your employees or family? Because of the lengthy periods without symptoms, thorough and frequent handwashing is particularly important. The best-practice solution includes vaccination.
With the quality defined, this operationally specific standard becomes the specification for your Ready-To-Serve Hand™. These are hands, bare or gloved, that are not likely to transfer an infectious dose of pathogens that cause foodborne illness. They are hands that are continuously returned to safe levels of bacterial and viral contaminants through processes that insure proper handwashing, sanitizing and gloving in terms of frequency, technique and materials used. Bare hands will always have some level of bacteria, as resident bacteria are part of our immune system. Transient bacteria and viral contaminants are common. Neither hands nor gloves can be sterilized. Monitoring actual levels of pathogens is not technically practical. The Ready-To-Serve Hand is normally one that has been recently washed. Additional interventions of sanitizing and gloving provide added levels of safety.
Good process management in hand hygiene begins with establishing what is acceptable behavior at the individual level in a food operation. Acceptable behavior is established, trained and managed in two parts: the quality of handwashing skills (how to wash) as discussed above, and the frequency of handwashing activity (when to wash). A common excuse when it comes to managing hand hygiene has been “management’s inability to police individual adherence” to documented policies and procedures. The truth is that most foodservice operators have yet to establish standards for either the quality of the wash or the frequency required. Those who offer hand hygiene training to employees often focus on the “why and how to wash” and then conveniently ignore managing the “when to wash” issue because normalized targets are almost impossible to apply and to enforce. This has been influenced by the regulatory pressure to wear gloves, as it is easier for a visual check during their brief visit. “When to wash” targets can only be accurately determined by knowing the overall operating risk, the task being performed and the individual employee. Wash frequency targets are as unique as the individuals to which they apply.
The primary qualification to establish the safe level for the frequency of handwashing is a thorough understanding of the food flow and the ability to convert findings from the risk assessment into a meaningful number. How many handwashes are required per shift by each person, and collectively, by the total number of people on the specific shift? Handwashing is not a function of time. It must be activity-based. It is critical to connect employee behavior with their impact on outcomes. Time masks the understanding of both why and when to wash. Washing once per hour by the clock alone can give a false sense of security and minimize the importance of avoiding hand-soiling occasions.
Step 3: Optimize Processes, Equipment and Supplies
Employees cannot be blamed for poor hand hygiene practices in a foodservice environment if standards are not set, agreed and communicated through training. Poor hand hygiene is primarily a management problem. Is there adequate process control for the handwashing system? Is there a written and documented system? Improving hand hygiene practices is not a one-time event. It requires commitment to continuous review and a disciplined routine by the PIC.
Achieving the level of commitment required for success is practically impossible without supportive management tools. This is the role of good policies and ingrained processes. When proper policies and processes are established there is a high probability that best-practice behavior will follow. The right processes keep important priorities like hand hygiene and food safety at the top of the PIC’s “to do” list.
“Best practice” equipment and supplies help make good hand hygiene behavior easy for employees. Handwashing that isn’t convenient, isn’t easy and isn’t comfortable, isn’t done. Likewise, products that leave hands irritated and rough aren’t used. Inadequate attention to equipment and supply details can actually result in handwashing avoidance. Take the necessary actions to insure that facilities, equipment and supplies are not deterrents to the success of employee training and motivation programs.
If your handwash stations are less than ideal get started on a continuous improvement program. While it is nice to have the latest and best of equipment, great improvements can always be made in handwashing practices using existing facilities more effectively. Often minor changes and/or additions can have a dramatic impact on employee use. Here are six recommended quick fixes to get started, using a basic list of equipment and materials that should be a part of any good handwash station system:
• Soap Dispensers: Eliminate any open-top soap dispensers because they can harbor microbes and/or be a source of contamination. Install a closed-bag soap dispensing system that comes equipped with a device for counting the number of times it is used. A counter is critical to provide management with a means for establishing and monitoring proper handwash performance.
• Towels: Wet hands readily transfer pathogens to food, utensils and other surfaces. Eliminate all blow dryer systems from employee handwash stations. Research has demonstrated hot air drying is counter to good hand hygiene practices. Select and install single-use paper towels that deliver soft, fast, one-sheet drying results. Install touch-free towel dispensers (i.e., no levers, buttons, dials to touch). When hands-free dispenser is not available, clean the dispensing parts frequently and sanitize with a good surface sanitizer.
• Hand Sanitizers: Install hand sanitizing stations in kitchen areas where it is not currently practical to install a full handwash station with water and drainage facilities. Also, ensure that wait staff have access to hand sanitizing stations at or near their work areas.
• Water: Ideal water is heated to 100ºF and flowing at a 2 gallon per minute (gpm) rate. Temperature is critical to encourage frequency of washing; flow is critical for effective washing. Take corrective action if the temperature is not comfortable. Also, consider hand sanitizer and a towel dispenser if warm temperature cannot be delivered to the station.
• Nail Brushes: Often, nail brushes harbor more microbes and pathogens than any other appliance in the kitchen. Dispose of high-risk brushes (i.e., wooden based, glued or stapled bristles, chained to sink, etc.) and replace with fused bristle brushes. Send these through the dishwasher frequently to sanitize them.
• Sinks and Faucets: In an existing operation it is often difficult to replace these basic fixtures. Ensure that any renovation takes the best technology into consideration. If you currently have faucets with hand-operated taps or buttons consider replacing them with automatic faucets or retrofitting with a hands-free or low-touch appliance. At a minumum, try to replace highly grooved taps with smooth surface taps for easy cleaning and sanitizing. If taps are your only option, ensure that surfaces are cleaned and sanitized regularly during the shift. Consider placing a surface sanitizing spray bottle at each handwash station. Also, teach employees to use hand towels when turning off faucets to prevent cross-contamination.
In general, a handwash station should be within three to four steps of all workstations in the kitchen. This is difficult to change in an existing facility, but proper design should be a priority in any renovation. Short-term, consider hand sanitizer and towel dispensers in areas underserviced by handwash stations.
Step 4. Train & Motivate
The responsibilityof every PIC in a foodservice operation is to ensure that all foodservice workers practice a safe level of hand hygiene. To achieve this without a structured and disciplined approach to training is practically impossible. Research in all regions and in most all types of foodservice environments continues to prove that hand hygiene practices are seriously inadequate. Managers and workers don’t understand the why, when and how basics of proper hand hygiene.
Knowledge is the key to understanding and is the primary driver in behavior change at the worker level. Behavior won’t change until every worker can demonstrate:
1. Why handwashing is important
2. The impact of a foodborne illness on their job
3. When they should wash their hands
4. The nature and resilience of foodborne pathogens
5. How they should wash their hands
6. The basic skills of washing, brushing, sanitizing and gloving
Training should include the clear communication of company handwashing policies, employee responsibilities and management responsibilities. For example, a company might communicate the following during training:
Employee Policy. “As managers and employees of ABC Foods we are responsible for the safety of our customers and fellow employees. We recognize that foodborne pathogens can be a serious problem leading to illness and death. We are committed to minimizing the risk of foodborne illness by adhering to best practices in personal hygiene and handwashing.”
Employee Responsibility. “Employees are responsible for using safe food handling methods as trained and instructed, and for practicing good personal hyg-iene including good handwashing. Emp-loyees must be able to describe and demonstrate these procedures and practices.”
Management Responsibility. “Managers are responsible for ensuring that emp-loyees are trained in safe food handling methods, that safe hygiene management processes are followed and that facilities are equipped and supplied with products meeting best practices criteria.”
Step 5. Monitor Performance
The hard work of Steps 1-4 is now complete. The risk of foodborne illness has been assessed and actions taken to manage the key factors. Hand hygiene frequency targets have been established at individual and team levels. Optimization of processes, equipment and supplies is progressing based on a prioritized plan, and all employees have been trained. Now, the performance of the system needs to be monitored to ensure that the best-practices approach is really paying off in reduced potential foodborne illness risk.
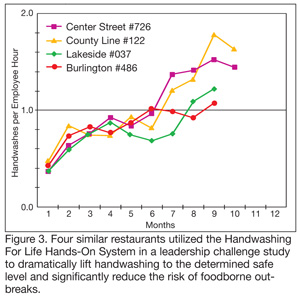 For example, this system was applied in pilot study of a full-service restaurant, five school cafeterias and a casual dining group. Eight restaurants serving the same menu were included as a separate research project, with results showing that following the implementation of the Hands-On program, their operations clearly achieved target safe levels for handwashing (Figure 3). Baseline comparisons were established in two geographic areas with handwashing rates clustered around the rate of 0.5 handwashes per employee hour. The first phase of hand hygiene program enhancements were largely attributed to the management’s attention to the subject and team training sessions conducted at each location. The second major gain resulted from a Team Tally Challenge where the four managers and their teams competed by collecting and sharing their rates.
For example, this system was applied in pilot study of a full-service restaurant, five school cafeterias and a casual dining group. Eight restaurants serving the same menu were included as a separate research project, with results showing that following the implementation of the Hands-On program, their operations clearly achieved target safe levels for handwashing (Figure 3). Baseline comparisons were established in two geographic areas with handwashing rates clustered around the rate of 0.5 handwashes per employee hour. The first phase of hand hygiene program enhancements were largely attributed to the management’s attention to the subject and team training sessions conducted at each location. The second major gain resulted from a Team Tally Challenge where the four managers and their teams competed by collecting and sharing their rates.
The biggest variable observed in the results was the quality of implementation. The better the manager, the better the result. According to the study, the single most difficult step for participants was securing adequate windows of time in which to get everyone trained. In some cases, team training was limited to about 50% of the staff. The remainder were trained individually but with little control of the method. This indicates the potential need to—and benefit of—including preliminary handwashing training within the hiring process.
What do you do when performance monitoring indicates poor practices? Performance that occasionally does not meet frequency targets should be addressed immediately by the PIC and a dialogue should be initiated on why performance does not meet the target and what options exist to correct the problem. Remember that not all issues are employee issues; some are related to problematic design, equipment and supplies. The occasional lapse in performance is often a result of workload and convenience. Performance that consistently fails to meet frequency targets should be addressed by the PIC and senior manager/owners. First, revisit the steps to look for oversights in the implementation process, and then meet with workers to discuss the issue and the course for improvement.
In addition to the importance of monitoring performance and troubleshooting poor performance, it is vital to recognize excellent employee performance of these best practices. Progress in improving hand hygiene practices doesn’t occur, and cannot be sustained, in the absence of an effective recognition system. The best recognition systems address all levels of individual and team performance, including:
• Performance that consistently exceeds frequency targets must be recognized by both the PIC and senior managers/owners. Use existing recognition tools to highlight performance (i.e., newsletters, bulletin boards, websites, staff meetings, bonus pay, etc).
• Performance that meets and occasionally exceeds frequency targets should be recognized by the PIC, with particular attention given to those times when goals are exceeded.
This suggested Hands-On solution offers many alternative paths for success in building a program of continuous improvement. The more thorough, the more enduring are the gains in hand hygiene and the reduction of operator risk.
Jim Mann is the founder and Executive Director of the Handwashing For Life Institute and the Handwashing Leadership Forum (www.handwashingforlife.com). His work to reduce the risk of foodborne illness spans a career from deli and cafeteria experience to work as a chemist. Earlier this year, Jim was honored as the recipient of NSF’s prestigious Lifetime Achievement Award for his contributions. Contact Jim at jmann@handwashingforlife.com.




