In previous decades, bacterial food poisoning was synonymous with the genus Salmonella. While Salmonella species are still responsible for a large number of outbreaks of foodborne disease, Campylobacter are now the most common bacteria associated with food poisoning and contamination in the European Union, the United States and, to an unknown extent, in the developing world, where detection and recording of infections is more limited. Bacterial food poisoning is particularly troublesome in impoverished countries where poor hygiene provisions correlate with a rapid spread of infection through contaminated food and water supplies. In the UK, Campylobacter infections are thought to cause more than 100 deaths per year, with many more people experiencing disease symptoms and decreased quality of life.[1] As a result, this pathogen is thought to cost the UK economy upward of £900 million per year. That’s enough money to build a brand-new NHS (National Health Service) hospital every year if we were to eliminate Campylobacter-associated disease. While this infection rate is primarily due to the undercooking and spread of contaminated chicken throughout the household, there is also a significant contribution from high levels of Campylobacter contamination on food packaging at the retail level, a problem that further propagates the spread of Campylobacter.[2] Novel strategies to prevent Campylobacter from entering the food chain, as well as to reduce the risk of contamination of other foodstuffs, are therefore a major priority. Progress in this area is hampered, however, by our limited understanding of the fundamental workings of this bacterial species at a genetic level.
At the University of Leicester (UoL), we have a long-standing interest in microbial sciences and, in particular, the under-recognized food superpathogen Campylobacter jejuni. In the Department of Genetics, made famous for the discovery of DNA fingerprinting by Sir Alec Jeffreys, we now have two active research groups interested in this organism. Understanding the genetics underpinning the disease-causing potential of Campylobacter is crucial. This article reviews how studies of the motility and mutability of C. jejuni at the UoL are advancing our understanding of the behavior of this bacterial species and could lead to improvements in food safety and disease prevention/control.
Campylobacter: Adapted for Survival
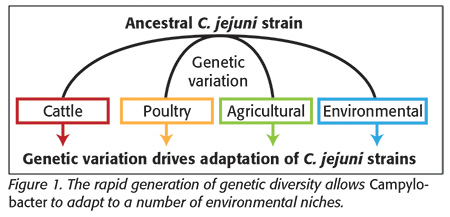 Campylobacter are spiral-shaped bacteria, very similar in size and structure to the gastric cancer-causing bacterium Helicobacter pylori. Campylobacter occupy several niches, which serve as bacterial reservoirs and are in direct contact with humans. This species is found in environmental niches such as riverine water sources or agricultural land as a result of treatment or contamination with fecal material from agricultural animals or wild birds (a natural host). The major sources for disease, however, are meat products from farmed animals, mainly pigs, cattle and poultry. The last of these species is the most important in the context of human disease due to the combination of high consumption and significant levels of bacterial cells in fecal excretions. Each niche mentioned above offers diverse challenges for the bacteria, with specific nutrient sources and differing physiochemical conditions. Transmission of Campylobacter between these niches exposes them to rapid fluctuations in stressful conditions. These pressures have resulted in the evolution of mechanisms in Campylobacter for the rapid generation of diversity that enables adaptation to and survival in a number of environments (Figure 1). This diversity is generated through several mechanisms, one of which (phase variation, PV) will be discussed in detail below.
Campylobacter are spiral-shaped bacteria, very similar in size and structure to the gastric cancer-causing bacterium Helicobacter pylori. Campylobacter occupy several niches, which serve as bacterial reservoirs and are in direct contact with humans. This species is found in environmental niches such as riverine water sources or agricultural land as a result of treatment or contamination with fecal material from agricultural animals or wild birds (a natural host). The major sources for disease, however, are meat products from farmed animals, mainly pigs, cattle and poultry. The last of these species is the most important in the context of human disease due to the combination of high consumption and significant levels of bacterial cells in fecal excretions. Each niche mentioned above offers diverse challenges for the bacteria, with specific nutrient sources and differing physiochemical conditions. Transmission of Campylobacter between these niches exposes them to rapid fluctuations in stressful conditions. These pressures have resulted in the evolution of mechanisms in Campylobacter for the rapid generation of diversity that enables adaptation to and survival in a number of environments (Figure 1). This diversity is generated through several mechanisms, one of which (phase variation, PV) will be discussed in detail below.
Campylobacter are potent pathogens due to their relationship with poultry and other birds. Most of our knowledge comes from studies of chickens and chicken flocks, whereas studies of wild birds are in their infancy. In many cases, the pathogens live “quietly” within chickens, causing no obvious symptoms of disease. Initial colonization of a chicken flock occurs when birds are about 2 weeks of age. Following a period of sustained growth, Campylobacter also become better adapted to colonizing these birds and spreading throughout the population.[3] This is critical, as it shows that Campylobacter can adapt to changing environments at the genetic level, a fact that has been supported by many scientific studies. Once they then make their way into the human gut, through ingestion of contaminated food, we have a problem. In the human gut, Campylobacter have several characteristics that adapt them to cause diseases such as gastroenteritis. At the UoL, we are interested in several disease-causing strategies of this pathogen, and how these strategies permit adaptation to different environments, with the goal of improving treatment/prevention strategies and, ultimately, food safety.
Motility and Chemotaxis of Campylobacter
Like Salmonella, Campylobacter can move toward nutrients in the gut and away from chemicals that may harm them. This ability relies on two processes, motility and chemical detection. When working together, these processes are known as “chemotaxis” and allow the bacteria to move in response to their chemical environment. This is crucial for Campylobacter to cause disease. In Campylobacter, propulsion for motility is provided by rotation of two thin fibers known as flagella[3] that extrude from both ends of the corkscrew-shaped cells. The motor for this structure is a large complex of proteins that span the cell wall and link the flagellum to the energy-providing proteins and control systems inside the cells. Campylobacter, in response to their chemical environment, redirect the rotation of their flagella through these internal systems and, subsequently, their movement. Chemotactic motility contributes to human disease by aiding high-level colonization of the avian gut and therefore increases the number of infectious cells that could make their way into our diets. Each chemical in the environment forms a chemotactic gradient, which determines the general direction of movement of the bacteria. When we observe Campylobacter moving in real time, we can see that they travel in a single direction (so-called runs) for a given period. They then randomly change direction and begin to move in another direction. So with these random changes in direction, how do Campylobacter ever migrate toward a favorable environment? The answer is that they will move further down a chemotactic gradient before changing direction than if they were moving up one (you can see a video of Campylobacter moving toward nutrients in real time on our website).[4] This process is governed by a complex cascade of reactions at the bacterial surface, which results in direct sensing of the chemical environment. One aim of Professor Julian Ketley’s research at the UoL is to unravel the molecular signaling events involved in taking external chemical signals from the gut and translating them into bacterial motility. Gradient detection in chemotaxis involves a series of “transducer-like molecules” that Campylobacter have in their inner membrane. These molecules have been shown to be responsible for sensing and converting the extracellular, chemical environment into a change in movement of the flagella.[5] Recently, we have shown that these molecules, while primarily affecting the chemotactic motility of Campylobacter, also diminish its ability to form clusters of cells known as biofilms when stimulated. Biofilms are involved in the persistence of the bacteria on abiotic surfaces, such as kitchen worktops or poultry waterlines, and so this chemotactic signal can switch Campylobacter cells into a motile (and hence infectious) mode, rendering them incapable of persistence on abiotic surfaces. This finding provides a platform for further understanding the ability of this pathogen to switch between a disease-causing state and one capable of persistence in the environment for long periods.
Currently, treatment for a Campylobacter infection focuses primarily on rehydration of the patient and later on antibiotic therapy in serious cases. A far more desirable approach would be to prevent colonization of the human gut by Campylobacter in the first place. In addition to motility, the Campylobacter flagellum is thought to be involved in adhesion (sticking) to the gut wall—a key initiator of infection and preceding the onset of Campylobacter-induced disease.[6] The chemical composition of the gut is in part determined by the food ingested by poultry. It may, therefore, be possible that alterations in the poultry feed could hamper the chemotactic motility of Campylobacter. If we can disturb the chemotactic motility of this bacterium, we may be able to perturb its colonization of poultry and prevent it from ever entering our food to begin with. Novel interventions such as this are essential in improving our food safety in the future, and an understanding of the underpinning genetics is key for this development.
Motility and Phase Variation: Hiding from the Host?
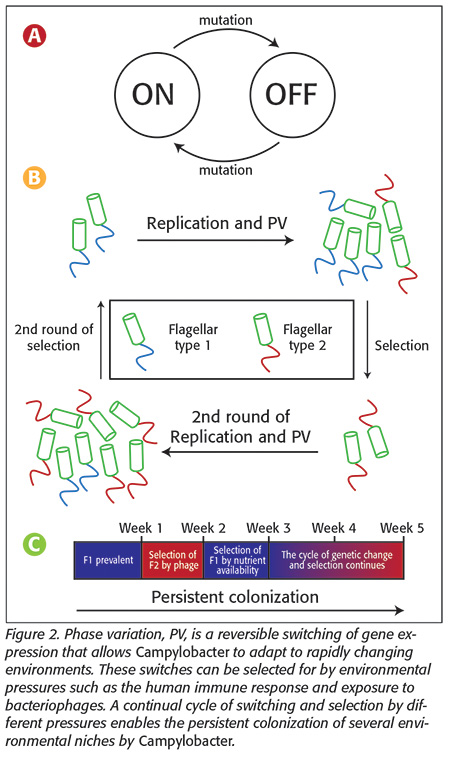 While motility is a key determinant of the ability of Campylobacter to cause disease, it can also be its Achilles’ heel. As with many other surface-exposed molecules, our immune system can recognize the bacterial flagellum as a foreign target antigen and help our bodies clear Campylobacter cells before they can multiply to high levels and cause disease. Unfortunately, Campylobacter have developed ways to hide the flagellum from our immune system, enabling these bacteria to escape the immune response and remain hidden in the gut. The flagellum is covered in short carbohydrates and other structures. These molecules are possible targets for immune attack, and therefore changing the forms of these structural decorations may hide the flagellum from the immune system. In some bacteria, including Campylobacter, the DNA code responsible for the enzymes that make these structures can mutate, preventing their formation on flagella. This process is reversible, meaning that another mutation in the opposite orientation can switch expression of the flagellin modification between an on and an off state. We speculate that this switching helps Campylobacter escape the immune system by switching cells between two states, one capable of inducing the immune response and one that isn’t (Figure 2a). As we can see in the example depicted in Figure 2, when Campylobacter replicates, it produces diversity in its flagella type. When the immune system, or bacteriophages (discussed below), responds however, some cells are capable of surviving the attack and proliferating. If the immune system targets and kills cells with the modification, then other, unmodified cells in the population may survive and proliferate to potentially cause future infections and disease (Figure 2b).
While motility is a key determinant of the ability of Campylobacter to cause disease, it can also be its Achilles’ heel. As with many other surface-exposed molecules, our immune system can recognize the bacterial flagellum as a foreign target antigen and help our bodies clear Campylobacter cells before they can multiply to high levels and cause disease. Unfortunately, Campylobacter have developed ways to hide the flagellum from our immune system, enabling these bacteria to escape the immune response and remain hidden in the gut. The flagellum is covered in short carbohydrates and other structures. These molecules are possible targets for immune attack, and therefore changing the forms of these structural decorations may hide the flagellum from the immune system. In some bacteria, including Campylobacter, the DNA code responsible for the enzymes that make these structures can mutate, preventing their formation on flagella. This process is reversible, meaning that another mutation in the opposite orientation can switch expression of the flagellin modification between an on and an off state. We speculate that this switching helps Campylobacter escape the immune system by switching cells between two states, one capable of inducing the immune response and one that isn’t (Figure 2a). As we can see in the example depicted in Figure 2, when Campylobacter replicates, it produces diversity in its flagella type. When the immune system, or bacteriophages (discussed below), responds however, some cells are capable of surviving the attack and proliferating. If the immune system targets and kills cells with the modification, then other, unmodified cells in the population may survive and proliferate to potentially cause future infections and disease (Figure 2b).
One result of this reversible switching phenomenon is that populations of Campylobacter, all theoretically arising from a single bacterial cell, may have different flagellum structures expressed on the surface. This switching of expression and subsequent generation of diversity—termed “phase variation” (PV)[7]—maximizes the chance that a population of Campylobacter cells will be able to survive in a niche and potentially cause disease. Our work at the UoL aims to better understand the role of PV in enabling Campylobacter to persist in poultry and to colonize the human gastrointestinal tract while avoiding the chicken or human immune responses.
Phase Variation: Implications for Bacteriophage Therapy
In addition to a role in motility, PV affects several other aspects of Campylobacter biology that may hamper our attempts to develop new prevention and treatment strategies. In light of the ever-looming possibility of a post-antibiotic era of medicine, scientists are constantly pursuing new avenues for the treatment of infectious disease. It is not mere chance that the use of antibiotics such as ciprofloxacin as growth promotants in poultry coincided with the evolution of antibiotic resistance. If we are to preserve the life of our current therapeutic antibiotics, we must collectively minimize this spread by lowering our antibiotic use in poultry and indeed in treatment of human disease, which in turn may require alternative treatment strategies.
One such alternative treatment option—already used in countries such as Russia and Georgia—is the use of bacteria-specific viruses, called bacteriophages, to selectively kill the infecting pathogen.[8] These “phages” do not cause any damage to human cells, but upon contact with bacterial cells will infect them, replicate within them and cause them to burst, clearing the infection. Campylobacter are selectively preyed on by a wide array of phages, so this is in theory an entirely feasible option for either treatment of Campylobacter infection or preventive treatment of Campylobacter-infected poultry or Campylobacter-contaminated poultry products. Much like the use of antibiotics, however, this strategy is not foolproof, as Campylobacter can evolve to resist infection by bacteriophages, and one culprit is, once again, PV.
Phages infect Campylobacter by attaching to structures decorating the flagella and other similar structures on the cell surface. As a result, the sensitivity of Campylobacter to phage infection is determined by the “modification states” of these structures. The protein molecules within the bacteria responsible for these modifications are subject to PV, allowing Campylobacter to change their modification state to resist phage infection,[9] much like they evade the immune system. This allows them to resist a variety of host pressures and persistently colonize (Figure 2c). As these different modifications, in addition to mediating phage resistance, may also play a role in the ability of Campylobacter to cause disease, there is a trade-off between phase-on and phase-off cells having different survival or disease-causing modes. Dr. Bayliss’s group is interested in fully characterizing the roles of PV in phage resistance, with the aim of optimizing future therapies. For this treatment strategy to be viable, a detailed understanding of the genetics underpinning resistance is paramount.
Potential Roles for Phase Variation in Guillain-Barré Syndrome
 In rare cases (fewer than 1 in 5,000), gastroenteritis caused by C. jejuni can progress to the muscular condition Guillain-Barré syndrome (GBS), a flaccid, full-body paralysis that is fatal in roughly 2 percent of cases. GBS is an autoimmune disease in which the immune system attacks our own cells and affects particular cells of the peripheral nervous system that are heavily involved in movement. C. jejuni’s role in GBS stems from the similarity between one of its surface structures (in this case, the sugary layer surrounding the cell known as the LOS) and components of the human peripheral nerve cells. So similar are these components that exposure of the human immune system to C. jejuni cells can occasionally result in the induction of cross-reactive antibodies that target not only the bacterial cell but also nerve cells (Figure 3). This constant attack by our own immune system is responsible for the symptoms of paralysis experienced by the patient. Despite the potentially lethal nature of GBS, our understanding of the disease and the role of C. jejuni in its onset is still relatively poor.
In rare cases (fewer than 1 in 5,000), gastroenteritis caused by C. jejuni can progress to the muscular condition Guillain-Barré syndrome (GBS), a flaccid, full-body paralysis that is fatal in roughly 2 percent of cases. GBS is an autoimmune disease in which the immune system attacks our own cells and affects particular cells of the peripheral nervous system that are heavily involved in movement. C. jejuni’s role in GBS stems from the similarity between one of its surface structures (in this case, the sugary layer surrounding the cell known as the LOS) and components of the human peripheral nerve cells. So similar are these components that exposure of the human immune system to C. jejuni cells can occasionally result in the induction of cross-reactive antibodies that target not only the bacterial cell but also nerve cells (Figure 3). This constant attack by our own immune system is responsible for the symptoms of paralysis experienced by the patient. Despite the potentially lethal nature of GBS, our understanding of the disease and the role of C. jejuni in its onset is still relatively poor.
However, it is known that one of the surface structures of the bacteria responsible for inducing GBS is phase-variable. Recently, our group has measured the rate of on and off switches in expression of this surface layer, and we are now trying to determine how this switching rate influences the onset of GBS. We are also looking at how often these changes occur in poultry and humans to understand whether changes in these GBS-promoting structures are helping the bacteria survive in these organisms. Currently, only two licensed immune therapies exist for the treatment of GBS, both of which are relatively successful at halting progression of the disease. Further understanding of the potential advantages of the different GBS-linked, phase-variable states in a range of environments (e.g., chicken cecum versus human intestine), as well as the factors involved in controlling the rate of PV, could lead to improvements in treatments to retard progression of GBS, and perhaps even to new strategies to circumvent or possibly even prevent the disease.
Phasotypes and the Phasome
As discussed above, PV can contribute to the variation of individual characteristics in Campylobacter (i.e., phage resistance, immune evasion). Each character-altering state is referred to as the bacterium’s “phase state.” While studying phase states as discrete entities is helpful for understanding the contribution of specific characteristics to the disease-causing potential of a cell, it is becoming apparent that we need to study the consequences of all the different combinations of phase states of all the phase-variable genes in each cell—something we refer to as the “phasotype.”[10] To set into context the enormous diversity generated by PV, a Campylobacter bacterium with 27 phase-variable genes can give rise to 227 independent phasotypes, which may each act differently during infection.
Here at the UoL, we are attempting to characterize changes in phasotypes in response to fluctuations in the local environment and sizes of Campylobacter populations. Studies in other bacteria have indicated that a single cell may be responsible for causing a bacterial infection. As the disease population arising from this single cell will be closely related, we refer to this as a bottleneck, which removes all the genetic variation in the population. Recently, we have discovered that imposition of a single-cell bottleneck on populations of Campylobacter can generate populations with differing phasotypes. If each of these phasotype patterns had a different outcome, say, sensitivity or resistance to immune effectors, then these small bottlenecks could produce person-to-person variations in disease outcome, something that may shift the current paradigm on treatment of infection and the use of personalized medicine.
Another key discovery arising from studying the DNA of multiple organisms is the extent of variation between different Campylobacter strains and species in the composition, number and type of phase-variable genes they contain. We refer to this variety of phase-variable genes as the “phasome,” and we have observed that phasome patterns are indicative of the evolutionary lineage of strains and the adaptation to different environmental sources of the bacteria. This latter feature implies that selective pressures may play an important role in determining the makeup of a population in differing environments and that certain phase-variable genes may be advantageous in a specific environment. In the context of food safety, an “-omics” approach to understanding variability is key, as this indicates the forces shaping the biological features of the organism and where interventions can be targeted.
Genetic Variation and Vaccine Development
In the era of modern medicine, vaccines have saved countless lives by halting the progress of infection by pathogens. Despite exhaustive research in recent years, there is not yet a licensed vaccine to prevent Campylobacter-induced disease or to reduce levels at the source (e.g., in chickens). This is due to myriad factors. Firstly, we have a poor understanding of the bacterium’s ability to cause disease. Despite its ubiquitous presence, we still have very little idea about how Campylobacter colonizes the gut, persists in the host and causes invasive disease. Secondly, as described above, Campylobacter can generate huge diversity through PV and other undiscussed genetic mechanisms. Finally, it is thought that although vaccines against Campylobacter may prevent conditions such as gastroenteritis, they may not prevent the human immune system’s reacting to the pathogen and the subsequent onset of GBS and reactive arthritis. This uncertainty only further reiterates the need for a better understanding of the biology of this highly relevant microorganism. Only through an understanding of genetic variation can we successfully inform vaccine development.
While food safety in the UK is very good, continued research into the causative pathogens will only help in reducing the serious illnesses associated with food poisoning, particularly by the big player, Campylobacter. Specifically, the success of Campylobacter as a human pathogen is owed in part to its immense ability to diversify, and as such, those developing future therapeutic strategies should consider this with great care.
For more information on the work ongoing at the UoL, email us at the addresses below or message us via Twitter: @Leicester_Micro. Alternatively, see the Virtual Genetics Education Centre11 Microbial Sciences website for resources centered on Campylobacter biology and PV.
Joe Wanford (jw643@leicester.ac.uk) is a Ph.D. candidate at the University of Leicester, England, investigating the genetics underpinning antibiotic treatment failure and persistence of infection.
Julian Ketley, Ph.D. (ket@le.ac.uk), is a professor of bacterial genetics and the head of the Department of Genetics at the University of Leicester. He leads an active research group investigating Campylobacter.
Christopher Bayliss, Ph.D. (cdb12@le.ac.uk), is a reader in bacterial genetics at the University of Leicester. He leads an active research group investigating genetic variation in Campylobacter.
References
1. www.food.gov.uk/science/microbiology/campylobacterevidenceprogramme.
2. www.food.gov.uk/sites/default/files/campylobacter-retail-survey-final-report.pdf.
3. Jones, MA et al. 2004. “Adaptation of Campylobacter jejuni NCTC11168 to High-Level Colonization of the Avian Gastrointestinal Tract.” Infect Immun 72(7):3769–3776.
4. www2.le.ac.uk/departments/genetics/vgec/schoolscolleges/topics/microbial-genetics-1/infection/campylobacter-motility-in-real-time.
5. Hartley Tassell, LE et al. 2010. “Identification and Characterization of the Aspartate Chemosensory Receptor of Campylobacter jejuni.” Mol Microbiol 75(3):710–730.
6. Wassenaar, TM et al. 1993. “Colonization of Chicks by Motility Mutants of Campylobacter jejuni Demonstrates the Importance of Flagellin A Expression.” Microbiol 139(6):1171–1175.
7. Moxon, R et al. 2006. “Bacterial Contingency Loci: The Role of Simple Sequence DNA Repeats in Bacterial Adaptation.” Annu Rev Genet 40:307–333.
8. Carrillo, CL et al. “Bacteriophage Therapy to Reduce Campylobacter jejuni Colonization of Broiler Chickens.” Appl Environ Microbiol 71(11):6554–6563.
9. Sørensen, MCH et al. 2012. “Phase Variable Expression of Capsular Polysaccharide Modifications Allows Campylobacter jejuni to Avoid Bacteriophage Infection in Chickens.” Front Cell Infect Microbiol 2: 11.
10. Bayliss, CD et al. 2012. “Phase Variable Genes of Campylobacter jejuni Exhibit High Mutation Rates and Specific Mutational Patterns but Mutability Is Not the Major Determinant of Population Structure During Host Colonization.” Nucleic Acids Res 40(13):5876–5889.
11. www2.le.ac.uk/departments/genetics/vgec/schoolscolleges/topics/microbial-genetics-1/human-pathogens-1/campylobacter-jejuni.
Campylobacter jejuni: Understanding the New Food Superbug




