Recently I read an e-mail that came from a business associate that listed what were termed as “useful new words.” These are combinations of common words that create a new descriptive term. An example was “inoculatte,” which refers to an injection of an espresso beverage for a direct infusion of caffeine. As an espresso lover I found this quite humorous and decided to create my own useful new words. One of the words I came up with was “allergent,” which refers to a gentleman who is so irritating that he gives you a rash just by his presence.
While I was very impressed with my humorous creativity (I am certain that I am the only one), there are approximately 7 million Americans that probably are not. These are individuals who deal with food allergies, the physical maladies that affect them and the challenges of finding foods that are clearly labeled so that they can consume them safely. For this reason both houses of Congress recently passed the Food Allergen Labeling and Consumer Protection Act (HR 3684 IH). It is expected that President Bush will sign this Act into law.
Provisions of the Act
The Food Allergen Labeling and Consumer Protection Act, when signed, will go into effect Jan. 1, 2006 (concurrent with the trans fat labeling requirements) and will amend the Federal Food, Drug and Cosmetic Act (21 USC 343), Section 403. The amendment will provide several requirements for both food manufacturers and government agencies. Primary provisions of the act are the requirement of easy-to-understand labeling of allergen ingredients on food packaging; declaration of allergens present in flavoring, coloring or incidental additives; and a report to Congress by the Secretary of Health and Human Services detailing the following:
• Analysis of the ways in which foods are unintentionally contaminated with food allergens in the manufacturing process
• Advice on industry best practices that can be employed to prevent cross-contamination
• Description of advisory labeling (such as “may contain”) used by food manufacturers and descriptions by consumers of the type of advisory labeling they would prefer
• Statement of the number of food facilities inspected in the prior two years with a description of the number of non-conforming facilities, the nature of the violations and number of voluntary recalls, or assurances of proper labeling
• Proposal of rules to define and permit the use of the term “gluten-free” on labeling
• Improved collection and presentation of data, in conjunction with the U.S. Centers for Disease Control and Prevention (CDC) and the FDA Commissioner, on the prevalence of food allergies, clinical significance or serious adverse events and modes of treatment for food allergies
• Recommendations on research activities concerning food allergies
• Pursuance of Food Code revisions to provide guidance for preparation of allergen-free foods
• Provisions for technical assistance to state and local emergency medical services for the treatment and prevention of food allergy responses
What this means to the food industry is change in the way foods are labeled, increased inspection by government agencies and the likelihood of more regulation involving handling and production of foods in environments in which allergenic agents are handled. The industry will need to develop the discipline to implement an effective allergen control and labeling management strategy.
The Need for the New Act
There may be good reason for the new laws regarding labeling of products containing allergens or made in plants or on lines where allergens are handled. It is estimated that 2% of adults and 3% of children in the United States are affected by food allergies. More than 30,000 people are treated in hospital emergency rooms for food allergy related reactions and anywhere from 150 to 200 people die each year as a result of allergic reactions. Couple this with statistics on the number of product recalls related to allergen cross-contamination—from zero in 1988, to 35 in 1990, to 121 in 2000—and there is a definite indication that there is a need for further regulation.
Two of the causes of these illnesses, deaths and recalls are production cross-contamination and/or mislabeling by the producer, resulting in allergen adulterated products reaching the consumer. Increasingly, however, consumers indicate that they are confused by the use of ingredient names with which they are not familiar on food labels. Thus, they are not able to identify allergenic ingredients in the products they buy or use. The person with the dairy allergy or the parent with the dairy-allergic child knows that they must avoid milk. However, they may not recognize the need to avoid “whey” or “casein” in products. The new act will require the food to indicate the presence of the more common name “milk” in addition to the technical term “whey.” This may be done parenthetically after the technical term or may be done by way of a “Contains” statement (i.e., “Contains Milk”) in close proximity to the ingredient statement.
The food allergen-sensitive consumer is savvy and has an understanding of food manufacturing practices. They read labels and want clear communication so that they know what foods to avoid. They will also ask questions at restaurants to verify the contents of foods prepared for them. Clear labeling of ingredients will help consumers make better choices for themselves or for the family member who has a food allergy. These consumers tend to develop loyalties to trusted brands and are appreciative of clear no-nonsense labels. They may be confused by “May Contain” labels or indicators that the product was “Packed on the same line/in the same plant that handles (eggs, nuts, fish, etc.).”
Also, consumers are not appreciative when a product that they have previously purchased with the knowledge that it contains no allergens has now been reformulated to include an allergen to which they are sensitive. Remember, it is not just the individual who will avoid buying these types of products: The primary shopper avoids for the whole family, so the number of consumers avoiding your product expands with the size of the family.
Allergies and Intolerance
The cause of a true food allergy is the protein in a food item, typically the primary protein. Thus, persons with wheat allergy will react to gluten and persons with milk allergy will react to lactose. These proteins are heat stable, and therefore will not be eliminated by a cooking process. When an allergic individual comes in contact with the protein, typically through ingestion (although some will react to simple skin contact), the body has an immune mediated response because it sees the protein as a foreign substance that must be eliminated. There is a release of histamine that can cause symptoms as mild as itchy eyes or skin to more severe reactions such as nausea and difficulty breathing. The most severe reactions may result in potentially fatal anaphylaxis.
Anaphylaxis is a Greek word meaning “protection” and it may be the result of exposure to food, insect stings or medication. Many equate it with difficulty breathing but it may incorporate numerous symptoms and result in systemic failure. This means that there may be edema in the lungs or the brain or kidney failure. The usual treatment for allergic reaction is intra-muscular injections of epinephrine; however in some of the most severe anaphylactic reactions this is not sufficient and the reaction may be fatal.
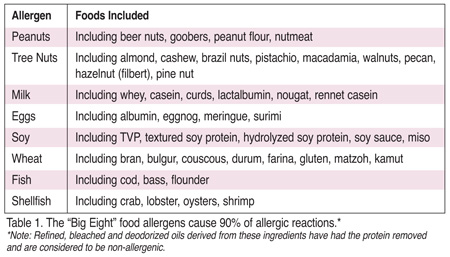 About 90% of all food allergy reactions come from specific foods referred to as the Big Eight (Table 1). Currently, there is no defined or consensus threshold level of protein that will cause a reaction. There are people with exquisite sensitivities that can react to presence of allergen protein at part-per-billion (ppb) levels. Therefore, any level of cross-contamination is considered as adulteration.
About 90% of all food allergy reactions come from specific foods referred to as the Big Eight (Table 1). Currently, there is no defined or consensus threshold level of protein that will cause a reaction. There are people with exquisite sensitivities that can react to presence of allergen protein at part-per-billion (ppb) levels. Therefore, any level of cross-contamination is considered as adulteration.
Persons with food intolerance have an enzyme deficiency that results in inability to metabolize certain proteins. Diseases such as Celiac Sprue, in which the person cannot metabolize gluten, or with lactose intolerance, the inability to metabolize lactose, do not cause life-threatening immune response. They do, however, cause symptoms that can range from mild discomfort to debilitating nausea. For food-intolerant individuals, as with food allergen-sensitive people, the best treatment is avoidance. They must rely on themselves to carefully read labels, and they must rely on food manufacturers to provide clear labeling and prevent cross-contamination.
Allergen Management
It is the primary responsibility of food manufacturers to provide safe foods, free from allergen cross-contamination. There must be a disciplined approach to allergen management. Depending upon the layout of the plant, ingredients handled and products made, each facility may have to incorporate different allergen management strategies. However, the following are basics that can be incorporated into any operation to provide an allergen-safe product:
• Adopt a “zero tolerance” philosophy for allergen cross-contamination.
• Conduct an allergen risk assessment as part of your Hazard Analysis and Critical Control Points (HACCP) program.
• Train all associates in allergen management strategy. Include Marketing, R&D, production, maintenance and sanitation.
• Make sure that incoming ingredients are clearly labeled and that the labels are reviewed periodically to assure suppliers have not changed ingredients without notice.
• Have a clear allergen storage policy including a procedure for spills cleanup.
• Design equipment to facilitate cleaning and prevent allergen harborage niches.
• Schedule production to prevent cross-contamination.
• Clean between runs of allergen ingredients. Use a visually clean standard or confirm with ezyme-linked immunosorbent assay (ELISA) test kits.
• Clearly identify work-in-process materials and rework. Have a clear rework policy.
• Reject in-process materials or finished product suspected of cross-contamination.
• Have a process for reviewing labels prior to use, and confirm that the correct labels are used in process.
• Conduct internal audits or use a third party auditor to assess the allergen management strategy.
• Evaluate and track consumer complaints involving allergen issues.
• Have a trained person on staff to respond to consumer calls regarding allergens.
Finally, be sure to provide consumers with quick, honest answers. One of the benefits of the Food Allergen Labeling and Consumer Protection Act to food manufacturers is that such good labeling practices let consumers know that you care and you want to help. I’d go so far as to say that this new act is “allergenius”; that is, a brilliant initiative in the food industry’s effort to educate consumers.
Michael M. Cramer, president of Cramer & Associates Food Safety Services, has spent more than 27 years in the food industry with such food manufacturers as Swift & Co. and Specialty Brands, and has experience with poultry and processed meats, batters and breaders, Mexican entrées, frozen appetizers and pasta. He has been responsible for development and implementation of food safety, quality and regulatory programs. Cramer has authored and spoken on the topics of biosecurity, sanitation, microbiological management, allergen management and quality programs. He is a Director with National Meat Association (NMA), serves on the Editorial Advisory Board of Food Safety Magazine and is a Professional Member of the Institute of Food Technologists (IFT).
Resources
There are tremendous resources available through the following noteworthy organizations, which can provide reference, scientific and support resources:
• Food Allergen and Anaphylaxis Network www.foodallergy.org/allergens.html
• Food Allergen Resource and Research Program, University of Nebraska www.farrp.org
• Institute of Food Technologists www.ift.org
• U.S. Food and Drug Administration Center for Food Science and Nutrition www.cfsan.fda.gov