A foodborne illness outbreak is like a ticking time bomb. With every minute, the risk to consumers and the secondary risk to industry is greater. What is the best way to defuse the time bomb? Could the answer be as simple as collaboration and information sharing? For the U.S. Food and Drug Administration (FDA) and the state agencies around the country that have created foodborne emergency Rapid Response Teams (RRTs), the answer is a resounding “Yes!”
It is no secret that fighting foodborne illnesses is a great challenge. The impact of an outbreak on public health is huge, as evidenced by the large outbreaks in the late 1990s into the early 2000s, culminating in the 2006 outbreak of Escherichia coli in spinach and the 2007 outbreak of botulism from Castleberry canned chili sauce that left 205 sick and 3 dead.
In fact, a 2011 report from the U.S. Centers for Disease Control and Prevention (CDC) reported an estimated 9.4 million episodes of foodborne illnesses each year in the U.S. from known pathogens. An additional 38.4 million cases are estimated to come from unspecified or unknown pathogens. In total, foodborne illnesses are thought to contribute to 48 million illnesses annually, resulting in more than 128,000 hospitalizations and 3,000 deaths.
The challenge is not unique to government, but is faced by industry as well. Foodborne illness outbreaks have a huge economic impact. Foodborne illness is estimated to cost the U.S. more than $14 billion annually, according to a 2012 report from the Emerging Pathogens Institute, Resources for the Future and the U.S. Department of Agriculture (USDA)’s Economic Research Service. This estimate takes into account factors such as medical costs and productivity losses.
Beyond the economic impact, there is an additional risk to industry that is not as easy to document but exists just the same.
“Nothing jeopardizes a food company’s ability to recover from a foodborne incident more than the loss of consumer confidence,” said Erik Oliver, senior research associate at Georgia Tech Research Institute during a recent industry workshop. “An incident at one company can have cascading effects on a whole commodity industry as well as further processing of foodservice companies that depend on key ingredients.”
With so much at stake, time is of the essence for the more than 3,000 federal, state and local government agencies that have regulatory authority over food at some point in the farm-to-fork continuum. The same is true for those agencies involved in disease surveillance and identification of foodborne illness outbreaks, including epidemiologic and laboratory investigations of human illness.
In recent years, federal, state and local agencies have shifted their thinking toward the concept of building an integrated food safety system. This food system should be capable of efficiently sharing information and resources across jurisdictional boundaries.
Integrated efforts would better identify suspected food vehicles and lead investigations to pinpoint and control sources of contamination faster. These efforts would protect all stakeholders against food safety and defense threats.
But how could this concept become reality? It could be done by creating mechanisms to allow participating agencies to share information in real time. Another solution could be creating a common operating picture and making decisions together, such as:
• Where do we focus resources?
• Which agency is best suited to provide resources for different aspects of the response?
• How can regulatory authorities leverage each other to quickly implement effective control measures?
 FDA recognized this need and created a cooperative agreement with nine states to develop and pilot food protection RRTs. These teams, composed primarily of FDA and state personnel, are resources dedicated to conducting rapid investigations of all-hazards food/feed contamination events (see Figure 1), identifying the source of the contamination and implementing effective control measures to protect consumers and mitigate the damage to the food industry.
FDA recognized this need and created a cooperative agreement with nine states to develop and pilot food protection RRTs. These teams, composed primarily of FDA and state personnel, are resources dedicated to conducting rapid investigations of all-hazards food/feed contamination events (see Figure 1), identifying the source of the contamination and implementing effective control measures to protect consumers and mitigate the damage to the food industry.
“Food safety challenges can never be completely eliminated as our food supplies become more global and diverse,” says Darla Bracy, deputy district director for the FDA San Francisco District Office, an active partner in the California Food Emergency Response Team (CalFERT). “We cannot solve food safety problems individually; we are stronger working as partners to combat the constant threat in food safety. As a Rapid Response Team, CalFERT’s mission is to protect public health by continuing to monitor, evaluate and respond to food and feed threats through coordination and collaboration with our multidisciplinary team of federal, state and local regulatory partners.”
These pilot programs immediately began improving food program infrastructure, strengthening collaboration and creating fully integrated and sustainable response capabilities for food emergencies. Today, the program has grown to 18 states and the concept has spread to other states that are not a part of the cooperative agreement with FDA.
“The real-world outcome of developing the RRT Program in 2008/2009 was to minimize the time between agency notifications of food safety threats and containing them,” says Carrie Rigdon, Ph.D., RRT supervisor of the Minnesota Department of Agriculture. “This protects public health. It mitigates negative economic impacts to the food industry and it restores the affected firm’s continuity of operations and consumer confidence. It defuses the foodborne outbreak time bomb.”
The Birth of RRT: Integrating a National Network for Response
Over the past 6 years, RRTs have focused on a continuous process-improvement approach to make the regulatory response to foodborne incidents more rapid and effective.
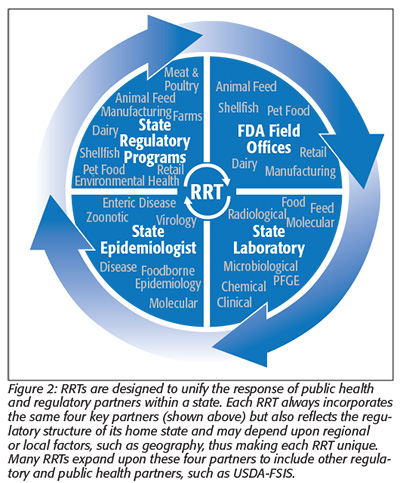 RRTs have worked to align preparedness, prevention, surveillance, response and mitigation efforts of the federal and state regulatory agencies within their states, including epidemiological and laboratory partners (see Figures 2 and 3). RRTs also work closely with the components of federal agencies responsible for coordinating the national regulatory or public health response for multi-state events. For example, during multi-state foodborne outbreaks, RRTs work with their FDA district office to receive updates on the national investigation and share the RRTs’ action plans and accomplishments with FDA’s Coordinated Outbreak Response and Evaluation (CORE) Network to ensure that the RRTs’ response activities are aligned with the national regulatory response. Similarly, state epidemiological partners of the RRTs work with the CDC’s Outbreak Response and Prevention Branch to receive and share information about the epidemiological investigation within the state and nationwide.
RRTs have worked to align preparedness, prevention, surveillance, response and mitigation efforts of the federal and state regulatory agencies within their states, including epidemiological and laboratory partners (see Figures 2 and 3). RRTs also work closely with the components of federal agencies responsible for coordinating the national regulatory or public health response for multi-state events. For example, during multi-state foodborne outbreaks, RRTs work with their FDA district office to receive updates on the national investigation and share the RRTs’ action plans and accomplishments with FDA’s Coordinated Outbreak Response and Evaluation (CORE) Network to ensure that the RRTs’ response activities are aligned with the national regulatory response. Similarly, state epidemiological partners of the RRTs work with the CDC’s Outbreak Response and Prevention Branch to receive and share information about the epidemiological investigation within the state and nationwide.
 “While each group has distinct roles in a food incident, many have overlapping authorities over the same products or companies, and everyone needs to work together to successfully complete the investigation,” says Mark Buxton, M.A., RRT program manager of the Missouri Department of Health and Senior Services. “This alignment makes that happen.”
“While each group has distinct roles in a food incident, many have overlapping authorities over the same products or companies, and everyone needs to work together to successfully complete the investigation,” says Mark Buxton, M.A., RRT program manager of the Missouri Department of Health and Senior Services. “This alignment makes that happen.”
Additionally, the RRTs have created improved and innovative methods for sharing information.
“Information sharing is crucial. Whether we are sharing data or our analysis, or training together or sharing lessons learned, communication links us together and makes the whole greater than the sum of its parts,” says Ernest Julian, Ph.D., chief, Office of Food Protection, Rhode Island Department of Health.
An important communication link for the RRT program is its yearly face-to-face meeting to discuss past response efforts, share response methods and train on different commodity investigation procedures.
The meeting’s participants include staff from all 18 RRT states, their FDA district offices, FDA’s Office of Partnerships, CDC, FDA CORE Network, FDA Center for Veterinary Medicine, FDA Office of Crisis Management, USDA Food Safety and Inspection Service (FSIS) and other experts. These meetings allow the RRTs to interact with one another, strengthen the network and introduce new states to the RRT process. In addition to the national annual meeting, individual teams host quarterly and yearly meetings, meaning that members of each state’s RRT are routinely training and working together. In some areas of the country where multiple RRTs are clustered together, RRTs hold regional meetings.
Mentorship: Paying Experience Forward
RRTs have also developed a mentorship program, in which teams established in the earlier iterations of the RRT program (circa 2008 and 2009) mentor the newer teams (added in 2012) through the team development process.
The mentoring program matches newer RRTs with another state, similar in regulatory structure, so the new RRT can build off their lessons learned from exercising response and information sharing during an investigation, as well as mature RRTs’ systems for training and team organization.
“The benefits of the RRT model have been proven many times over and are a fantastic example of the integrated food safety system in action,” says Barbara Cassens, acting director, FDA Office of Partnerships. “It has been extremely rewarding to witness the growth of the program from 6 states in 2008 to 18 states in 2015, and even more rewarding to see how the original RRTs have taken the newer RRTs under their wing, really taking their role as mentors to heart.”
The mentoring program extends to nonfunded RRTs as well. The original RRTs have reached out upon request from nonfunded RRT states to provide an overview of the RRT program. FDA is developing a nonfunded RRT guide to getting started so all states can create an RRT program appropriate to their level of interest and available resources. These nonfunded states are recognized as an RRT and invited to attend all RRT meetings and national program functions. The progression of the program to include nonfunded RRT expands the network and spreads the use of uniform standards and response practices.
“Providing mentorship and training to others, sharing expertise and experiences and bringing all stakeholders together takes a truly collaborative approach to outbreak and emergency response,” reflects Cassens. “These things are the foundation of the national RRT network, and without a doubt play a central role in the success of the program to date.”
Another means of sharing information, and a more passive form of mentorship, has been the RRT Best Practices Manual, available at www.afdo.org.
This manual is one of the most prominent accomplishments of the RRTs, listing all the resources the RRTs use to communicate, collaborate, train, improve and investigate. It features tools to be used for program improvement in several key areas of response, such as communication Standard Operating Procedures, traceback, joint investigations and inspections. The manual also establishes metrics for rapid response capabilities that allow RRTs to assess their status, identify improvement plans and quantify accomplishments and impact.
Updated periodically, the manual may expand to better address different levels of government, different industry sectors and commodities. Additionally, the manual may be modified to address different phases of response, such as surveillance, recovery or prevention. Updates may also address different threats, such as natural disasters or intentional contamination. The manual truly reflects the wealth of knowledge and subject matter expertise developed by these teams to date.
Stay Tuned
In the next issue of Food Safety Magazine, we provide real-world examples of the RRTs in action, tying together program and practice, framework and function, in a sequel article entitled “Where the Rubber Meets the Road: RRTs in Action.”
Special thanks: The authors want to recognize the contributions that Lauren Yeung and Doug Karas, both of FDA, made to this article. Their support and guidance were essential. We also thank all of the RRTs for their assistance in the creation of this work.
Jennifer Pierquet, M.P.H., senior project manager, Minnesota Department of Agriculture, Dairy and Food Inspection Division.
Mark Buxton, M.A., RRT program manager, Missouri Department of Health and Senior Services.
Jessica Badour, Recall Outreach Specialist, Georgia Department of Agriculture.
Ernie Julian, Ph.D., chief, Rhode Island Department of Health, Office of Food Protection.
Alida Sorenson, M.P.H., recall coordinator and RRT investigator, Minnesota Department of Agriculture, Dairy and Food Inspection Division.
Brian Sauders, Ph.D., RRT coordinator, New York State Department of Agriculture & Markets.
Creating the Rapid Response Road Map: Collaboration Points the Way Forward