New initiatives focus on allergens in 2001.
As part of the public health mission to keep food safe, the U.S. Food and Drug Administration (FDA) is increasing its activity on food allergen awareness. FDA’s 2001 allergen priorities for the Center for Food Safety and Applied Nutrition (CFSAN) describe new initiatives.[1] For example, a major goal is to provide guidance to industry and regulators on how to manage allergens through appropriate manufacturing and labeling practices.
For sensitive individuals, the presence of allergens in food is potentially life-threatening. Currently, there is no cure for food allergy. The only successful method to manage food allergy is avoidance of foods containing the allergen. Fortunately, most consumers are aware of their specific sensitivities and can avoid foods that might result in a life-threatening situation. For example, a person with a peanut allergy may find it easy to avoid whole peanuts. Formulated foods, however, present a separate challenge. In such cases, the individual relies on accurate ingredient labeling. The FDA, food manufacturers and special interest groups are working to increase public awareness of the seriousness of allergic reactions and to assure that allergens are appropriately labeled in food products.[2] For example, one of the U.S. Department of Health and Human Services’ “Healthy People 2010” initiatives for the coming decade is to reduce the number of deaths due to anaphylaxis caused by food allergens.[3]
Allergic reactions are reported to be caused by a large variety of foods, and in theory, any food protein is capable of causing an anaphylactic reaction.[4] Agency allergen awareness efforts currently focus on the eight foods that are most frequently implicated in serious allergic responses: milk, eggs, fish, wheat, tree nuts, legumes (particularly, peanuts and soybeans), crustaceans and mollusks.[1] Allergenic proteins in these eight foods are estimated to cause 90% of the allergic reactions in the U.S.5 Some of these foods, such as milk and eggs, are often used as added ingredients in formulated products. Low amounts of these proteins may elicit a response and reactions may vary from mild to life-threatening, depending on a person’s particular sensitivity. (Other substances, such as FD&C Yellow No. 5, sulfites and carmine/cochineal extract, also may cause allergic or allergic-type reactions.)
The number of allergic individuals in the U.S. is unknown. Estimates suggest, however, that 1.5% of the adult population and 5% of children younger than three years old have some form of food allergy.[6] One estimate of the number of fatal food anaphylaxis cases in the U.S. is 125 per year.[4]
 The Ingredient Label: Alert for the Allergy-Sensite Person
The Ingredient Label: Alert for the Allergy-Sensite Person
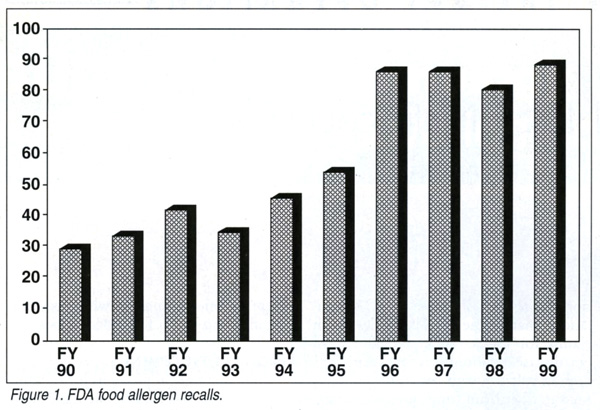
The Federal Food, Drug, and Cosmetic Act (FD&C) requires, in virtually all cases, a complete listing of all the ingredients of a food on the food label. In certain cases, such as with allergens, public health concerns have been noted as FDA took steps to require particular wording in an ingredient statement. For example, 21 Code of Federal Regulations (CFR) 102.22 requires the food source identification for protein hydrolysates, e.g. “hydrolyzed wheat gluten,” and “hydrolyzed soy protein.”7 Failure to list an ingredient on the food label, particularly an allergen, has resulted in product recalls. A recent review of FDA food recall actions for undeclared allergens such as peanuts, egg, or milk revealed an increase in recalls during the last decade. Recall activity increased from an average of 35 per year at the beginning of the last decade to an average of 90 per year during the last four years of the same decade (Figure 1).
Additionally, FDA has received a number of reports of consumers who experienced adverse reactions following exposure to an allergenic substance in foods. Many of these exposures occurred because the presence of the allergenic substance in the food was not declared on the food label. This public health concern has prompted FDA to develop an initiative on food allergen awareness.
In the spirit of the 1990 Nutrition Labeling and Education Act (NLEA), FDA’s activities during the past 10 years have encouraged consumers to read the product label. While it is understood that an added ingredient must be declared in the ingredient statement, food manufacturers must pay particular attention to instances in which inadvertent introduction of allergens can potentially occur because of the firm’s production practices; for example, rework addition, product carryover due to use of common equipment, production scheduling or allergenic product above exposed product lines.
In 1996, FDA issued a notice to the food industry alerting manufacturers and trade associations, requesting assistance in addressing the major public health problem of undeclared allergens in food.[8,9] FDA commented on current labeling requirements, voluntary labeling practices used by industry and various options such as additional rulemaking to alert consumers to the presence of allergens. In particular, the FDA noted the importance of declaring allergens even when present in very low amounts.
Collective Naming and Incidental Ingredients
The 1996 notice describing FDA’s policy for food allergens outlined “exemptions” under the law for the labeling of ingredients, including food allergens on food packaging, and noted the use of precautionary statements such as “may contain” on food ingredient labeling. The “exemptions” are of two types: One focuses on collective naming of spices, flavors and colors, and the other on declaration of incidental additives such as processing aids.[10,11]
The first exemption refers to collective naming of flavors, certain colors (color additives exempt from certification in 21 CFR Part 73) and spices. Although these terms may be used on the food label, they are not completely descriptive. Food labels with collectively named additives may confuse individuals who wish to avoid allergenic substances, particularly when the allergenic substance is not clearly labeled. On several occasions, the FDA has clarified publicly that the FD&C Act allows spices, flavors, and colors to be declared collectively without naming each one. In some instances, these ingredients contain subcomponents that are allergens. Therefore, FDA recommends that processors declare allergenic ingredients in a spice or in a flavor. This might be accomplished by either declaring the allergenic ingredient by its common or usual name in the ingredient list as a separate ingredient or parenthetically following the term spice, flavor or color, or as a separate declaration immediately below the list of ingredients indicating the presence of the allergen. In addition, for some food labeling decisions, it is also clearly advantageous to the allergic consumer for the manufacturer to voluntarily declare any allergenic source from which an ingredient may be derived, such as soy, milk and eggs.
The second “exemption,” incidental additives, refers to food substances that are exempt from labeling on an ingredient statement because they are used at or find their way into food at insignificant levels and do not have any technical or functional effect in that food. In this case, each individual food firm makes an assessment of the food ingredients that may be introduced during food processing into their final food product and then determines the ingredient label. This can lead to errors in judgment by the food industry or others involved in food handling as to what ingredients should be declared on the food label. While FDA believes that every food firm makes a sincere effort to label the ingredients in their food products completely, it is also clear that firms do miss including allergenic ingredients on their food labels. This happens at times because subtle changes in food processing aids, such as filtering substances, may introduce allergenic components into the manufactured food and a company may simply not realize the addition of such an allergen to the final food product. The agency stated in its 1996 notice that ingredients that are food allergens do not meet the requirements for incidental additives and therefore are not exempt from ingredient declaration. [8,9] When these labeling errors are found by consumers or the food industry, the food label is usually corrected. At times, these errors also result in a recall of a company’s products if they reach the marketplace.
Precautionary Labeling Statements
The 1996 notice also addressed the use of precautionary labeling statements. 8,9 Statements such as “may contain peanuts” or “made on shared equipment” are voluntarily placed on food packaging labels by food manufacturers. These statements tend to express the manufacturers’ concern that their food products could possibly contain other food ingredients not listed on the food label in the final food products. It is not clear whether the “may contain (ingredient)” is or is not present in this particular food package. The agency is gathering data on the extent of use of “may contain (ingredient)” and other precautionary labeling statements and intends to address their use in the future.
Food Allergen Initiatives and Policy Development
Beginning in 2000, CFSAN made increasing consumer and industry awareness to the presence of allergens in foods a high priority. In meeting the 2000 goal of increased awareness, CFSAN representatives held meetings at 14 locations in which they made presentations on allergen risks and labeling requirements.[12] CFSAN increased allergen awareness for those groups who provide food products to the public, as well for parents who may not be familiar with the challenges of caring for children who have a food sensitivity. These productive exchanges provided FDA with an opportunity to gather information for helpful consumer messages from individuals who, personally, or through their children, experienced allergic responses. For example, consumers suggested the use of certain terms to call attention to the presence of an allergen, i.e. use “milk” in the ingredient statement, if the formulation contains caseinate, or “egg” if the food contains albumin. The agency also sought to gain insight into industry allergen management practices and control methods. As part of the 2000 effort, FDA and state health departments began working cooperatively to establish uniform inspection procedures for food allergens.
Continuing these efforts with the 2001 CFSAN priorities, CFSAN plans to proceed with consumer and industry education efforts and to develop a strategy for clearer labeling of food allergens on the food label. Priorities include publishing a draft Compliance Policy Guide on manufacturing and labeling practices, issuing a field allergen inspection guide and providing training for FDA field offices. While emphasis is on the eight food allergens, FDA plans to publish a proposed rule to require declaration of carmine/cochineal extract on product labels.
Other Reserach Activities
Survey. A national assessment of the extent of food allergenicity would be helpful to clarify who and to what extent consumers experience allergic reactions to food. The agency is studying ways to accomplish this survey and is seeking suggestions from those who are interested. One approach that is being considered is to use eight or nine regions of the country to determine, through hospital emergency room discharge codes, how many people have food allergen problems and anaphylaxis during the course of a year and how much of this anaphylaxis is caused by food. Investigating hospital discharge codes has been discussed in medical literature, but these studies have involved only isolated parts of the nation.[13]
Food Allergen Test Kits. Detecting the allergenic protein components of the eight major allergenic foods is the subject of much research and development. The developers of tests that can detect minute levels of these proteins have to produce antibodies for these proteins from animal sources. Once an antibody is isolated, barriers such as cross-reactivity to substances other than the desired proteins have to be addressed. Results must be reproducible and kits must be effective to detect these proteins in different foods.
A number of test kits are manufactured in this country for commercial use. Although there is not a test kit for each allergen in the food supply, kits are available for peanut, milk and egg protein. Other test kits for allergenic proteins are under development. The FDA is participating with the National Food Processors Association (NFPA) in establishing a peanut protein standard. A peanut flour standard is being developed that will be used to establish a common relationship or scale for the peanut protein test kits currently on the market. Although plans include standard development for other allergenic proteins, much work is needed to develop test kits and common standards for these proteins.
Food Allergen Thresholds. As mentioned above, quantitative food allergen thresholds are currently unknown. Although available data suggest that it is not possible to determine the amount of allergenic protein necessary to elicit an allergic reaction, discussions in public forums offer the hope that future research will determine a safe level for undeclared allergens in food.[14] FDA welcomes receiving any human data that might be available to help determine possible limits for the effects of allergenic proteins in sensitive populations.
Other Initiatives
Importantly, FDA recognizes the efforts of the food industry in addressing the presence of food allergens. For example, major industry representatives are supporting CFSAN priorities and have signaled development of a voluntary allergen labeling program.[15] Industry’s senior management has made a commitment to managing allergens by training employees on allergens and plant-specific control procedures, evaluating rework procedures, working with ingredient suppliers to identify and label all allergenic ingredients in their products, requiring documentation of equipment cleaning and sharing best allergen practices with other corporations.
Information sharing among interested parties will go a long way to address the public health problem of food allergens. CFSAN anticipates that in 2001 public exchanges will continue through workshops as well as comments received on any guidance that issues. We look forward to constructive activities.
Kenneth J. Falci, Ph.D., is the Director of the Office of Scientific Analysis and Support, CFSAN, FDA. His office oversees development of economic impact analyses for food and cosmetic regulations, the conduct of consumer attitude studies including diet and disease, biotechnology and infant feeding practices. His office also provides epidemiological reviews for microorganism risk assessment, acute health hazard evaluations and estimates for the burden of foodborne illness. Post-market surveillance and adverse reactions to food products are also reported to his office.
Kathy L. Gombas is the Deputy Director of the Division of HACCP Programs, CFSAN, FDA. Her division provides technical expertise and leadership in areas of food safety programs and HACCP to support the development of agency policies, regulations, standards and training.
Elisa L. Elliot, Ph.D., is a microbiologist in the Division of HACCP Programs, CFSAN, FDA, with lead responsibility for the food safety portion of the 115. DHHS Healthy People 2010 initiative. She began her 11-year career with FDA as a researcher developing methods for Vibrio species.
References
1. U.S. FDA. 2001 CFSAN Program Priorities, p. 28. January 9, 2001.
2. Information on FDA’s activities and general information on allergens may be accessed at www.cfsan.fda.gov/~dms/wh-alrgy.html. The Food Allergy and Anaphylaxis Network provides valuable information to consumers at www.foodallergy.org.
3. U.S. Department of Health and Human Services. Chapter 10, Food Safety. In Healthy People 2010, 2nd ed. U.S. Government Printing Office (GPO). Washington, DC. November 2000. pp. 10-14.
4. Burks, A.W. and HA. Sampson. Anaphylaxis and food allergy. In Food Allergy: Adverse Reactions to Foods and Food Additives, 2nd ed. D.D. Metcalfe, HA. Sampson and R.A. Simon, eds. Blackwell Science. Cambridge, MA. pp. 246-247.
5. Hefle, S.L., et al. Allergenic foods. Crit. Rev Food Sci. Nutr. (36)5, pp. 69-89. 1996. www.cfsan.tda.gov/~lrd/allerg7.html
6. Sampson, HA. Food allergy. JAMA (278), pp.1888-1894. 1997.
7. Federal Register (58), p. 2850. Jan. 6, 1993.
8. U.S. FDA. Notice to Manufacturers. June 10, 1996. www.cfsan.tda.gov/~lrd/allerg7.html.
9. U.S. FDA. Letter from Commissioner of Food and Drugs. Dec.11, 1996.
10. Federal Food, Drug, and Cosmetic Act. Section 4030).
11. Code of Federal Regulations. 21 CFR ?101.100(3).
12. View “FDA Food Allergens and You,” a slide presentation by Kenneth Falci, Ph.D., at http://vm.ctsan.fda.gov/~comm/vltaller.html.
13. Yocum, MW., et al. Epidemiology of anaphylaxis in Olmsted County. J. Allergy Clin. Immunol. (104), pp. 452-456. 1999.
14. Hourihane, J. O'B., et al. An evaluation of the sensitivity of subjects with peanut allergy to very low doses of peanut protein: a randomized, double-blind, placebo-controlled food challenge study. J. Allergy Clin. Immunol. (100), pp. 596-500. 1997.
15. Grocery Manufacturers of America. Letter from L.D. Katic and J.H. Skiles to Director, CFSAN. Dec. 4, 2000.
>




