There is probably nothing that will make a person a food safety zealot more than a personal experience with a food safety hazard. About 10 years ago, I was working at one of our plant locations when a food safety/quality assurance tech offered me a plate of fruit. I accepted and eagerly consumed the delicious strawberries and slices of kiwi and mango. About 30 minutes later, I noticed that my hands were itching…which progressed to my neck…which progressed to my face…which progressed to sinus swelling and eye irritation.
Soon after these symptoms appeared, I made a trip to the plant clinic; the doctor concluded, based on the timing of the symptoms, that it was likely something on the fruit plate that I had eaten. As he began treatment, I learned two valuable things about medical procedures for allergic reactions: First, when the doctor says, “I’m going to give you a shot in your hip,” he really doesn’t mean your hip but a larger portion of the body in close proximity to the hip! The second thing I learned is that Benadryl is a very effective antihistamine that causes drowsiness; when the doctor recommends that you should not drive after taking it, don’t drive!
I didn’t really think much of it afterward but suspected that I had a reaction to the kiwi because I really don’t eat it very often and sometimes an allergic reaction can accompany foods that aren’t consumed very often. However, about a year later, I was home eating a mango that a friend had brought, and within 15 minutes of consumption, I started to have the same symptoms as before, only this time, I also noticed that my soft palate was starting to get firm and swallowing was difficult.
 This time, the trip was not to a clinic but to the emergency room, where I spent several hours hooked to an IV, given another dose of Benadryl and provided with an EpiPen, which I now carry with me (Figure 1).
This time, the trip was not to a clinic but to the emergency room, where I spent several hours hooked to an IV, given another dose of Benadryl and provided with an EpiPen, which I now carry with me (Figure 1).
It was now clear that I was one of almost 15 million Americans who have a food allergy and that I was reacting to mango. I found this surprising because I was very familiar with the “Big Eight” allergens, those foods that are responsible for the majority of food allergy responses, and mango is not included in that group. However, during a conversation with a colleague, I was informed that mango is related botanically to cashews, a tree nut that can result in an allergic reaction. Although I’m quite sure that I’m not allergic to cashews, considering I’m eating them as I write, I’m not willing to take any more chances with mangoes and do everything I can to avoid them.
For those with food allergies, avoiding exposure to the foods we react to is very important. However, as food manufacturers, we have an obligation to protect consumers, our customers and our companies from preparing foods that are either mislabeled and do not correctly declare the allergens that are present or that contain undeclared allergens due to cross-contamination. To do this, we need to understand the causes of food allergy reactions and how to prevent adulteration of our food products with undeclared allergens.
What Causes Food Allergies?
For some individuals, exposure to certain foods results in an allergic reaction by the body. It is the major protein in the food that the body identifies as a foreign invader when the food is consumed. The response is for the immune system to create antibodies called immunoglobulin E and release histamine, which can result in the symptoms of allergic reaction. These symptoms can be as mild as itchy eyes, runny nose or rash. However, more severe reactions can include difficulty breathing and anaphylaxis, which can be life-threatening. Anaphylaxis is severe and may result in the failure of the respiratory, nervous or hepatic systems, for example. The most severe cases of anaphylaxis can result in fatality.
 While many foods with proteins can result in allergic reaction in sensitized individuals, there are eight most commonly recognized foods that result in allergic reactions in the United States. These are referred to as the “Big Eight” and are shown in Figure 2. These foods are wheat, milk, fish, peanuts, soy, eggs, crustacean shellfish and tree nuts. Tree nuts include cashews, Brazil nuts, pine nuts, almonds, pecans, walnuts, hazelnuts, macadamia nuts, pistachios and coconuts. In addition, each different tree nut has a different protein, so if you are using multiple types of nuts, you must prevent cross-contamination by each type.
While many foods with proteins can result in allergic reaction in sensitized individuals, there are eight most commonly recognized foods that result in allergic reactions in the United States. These are referred to as the “Big Eight” and are shown in Figure 2. These foods are wheat, milk, fish, peanuts, soy, eggs, crustacean shellfish and tree nuts. Tree nuts include cashews, Brazil nuts, pine nuts, almonds, pecans, walnuts, hazelnuts, macadamia nuts, pistachios and coconuts. In addition, each different tree nut has a different protein, so if you are using multiple types of nuts, you must prevent cross-contamination by each type.
It is also important to remember that many of these allergens can be identified by different names. Soybeans can be prepared as tofu or edamame. Milk byproducts include whey or caseinate, and meringue is made of whipped eggs. The confusion that this can cause consumers resulted in the Food Allergen Labeling and Consumer Protection Act (FALCPA) of 2004. FALCPA requires that food labels bear clear information as to the contents of the product. This can be done either parenthetically or with a “contains” statement at the end of the ingredient listing. Consequently, a product formulated with the ingredient calcium caseinate may read “calcium caseinate (milk)” or may bear the statement “Contains Milk” at the end of the complete ingredient listing.
In Canada and the European Union (EU), additional foods have been identified as contributing to allergic reactions. In Canada, these include sesame and mustard seeds, whereas in the EU, the list includes celery, mustard, sulfites and lupine. If you manufacture and distribute product to Canada or the EU, it is wise to know the specific allergens that require labeling and control.
There are also foods that can cause reactions in people that are not immune system-mediated responses, that is, they do not cause a true allergic reaction. Celiac disease is a genetic disorder that results in symptoms caused by a reaction to gluten in grain that ultimately can damage the digestive system. Food intolerance is a sensitivity that does not involve an immune system response. An example is lactose intolerance, the inability to digest or absorb lactose, a sugar in milk, which results in gastrointestinal distress.
Other reactions to foods include sensitivity to sulfites, used to prevent oxidation in food, monosodium glutamate (MSG) and yellow food coloring. However, as more studies are conducted, there are findings that reactions to MSG and yellow food coloring may be idiosyncratic.
There is no identified lower threshold above which people with food allergies will react; consequently, reactions can occur with nothing more than dust (i.e., from peanuts or tree nuts) or residue from eggs, milk or fish. This is why there is a zero tolerance for cross-contamination of food products by undeclared allergens. Cross-contaminated or mislabeled foods in commerce will require a recall to prevent harm to people with food allergies.
How Do We Prevent Allergen Contamination?
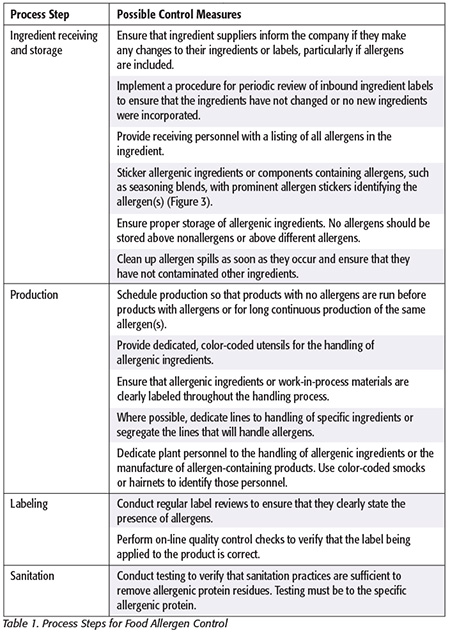 There are several means by which food manufacturers can prevent mislabeling or cross-contamination of their products. It is recommended that the facility map its process for handling allergens and determine points in the process where allergens can be controlled. An example of points in the process where controls may prevent allergen cross-contamination is provided in Table 1. An example of a prominent allergen sticker identifying allergens in a case of food products is shown in Figure 3.
There are several means by which food manufacturers can prevent mislabeling or cross-contamination of their products. It is recommended that the facility map its process for handling allergens and determine points in the process where allergens can be controlled. An example of points in the process where controls may prevent allergen cross-contamination is provided in Table 1. An example of a prominent allergen sticker identifying allergens in a case of food products is shown in Figure 3.

Training and Education
Even with the most thorough and well-designed process mapping to prevent allergen cross-contamination, the possibility remains that personnel will make mistakes, especially if they have not been trained or educated in food allergen management strategies. It is extremely important that all plant personnel receive specific and documented training regarding food allergen handling, particularly if this is or may be part of their assigned duties. New Food Safety Modernization Act (FSMA) regulations now require that allergen cross-contamination be included in company Good Manufacturing Practices. FSMA also requires that plant management ensures that all employees, including temporary employees, have received documented food safety training, including allergen training. An effective allergen management training and education program will be necessary to ensure that employees who receive and store allergenic ingredients, who handle allergenic ingredients in the manufacturing process, who label finished goods and who clean the plant can help prevent the cross-contamination and mislabeling of food products.
It is my hope that no one reading this article will ever have to go through an allergic experience the way I did. But I also hope that you and your food plant teams will become zealots for the prevention of allergen cross-contamination and mislabeling to protect consumers, prevent serious allergen-related hospitalizations and reduce the number of allergen-related recalls.
Michael Cramer, CQA, is the senior director, food safety and quality assurance, for Ajinomoto Windsor.




