“In a time of drastic change, it is the learners who inherit the future. The learned usually find themselves equipped to live in a world that no longer exists.” — Eric Hoffer
Our world as food scientists has changed already. The most recent Centers for Disease Control and Prevention Foodborne Diseases Active Surveillance Network Report of Incidence and Trends of Infection with Pathogens Transmitted Commonly Through Food (1996–2010) clearly highlights recent data indicating that reported illnesses associated with non-O157 Shiga toxin-producing Escherichia coli (STEC) are essentially equal to those attributed to O157:H7 STEC. Although trends were not assessed because of “sparse data,” the 2010 number is sufficient to justify the attention this group of pathogens is receiving.
Since the mid-1990s, we as food safety professionals have been focused on reducing or completely eliminating one specific STEC: E. coli O157:H7. Intense industry focus has resulted in impressive reductions in the prevalence of this deadly pathogen in the food supply and the work accomplished by the food industry should be cause for celebration. We cannot know the number of lives that have been saved and illnesses that have been prevented, but we can be absolutely certain that our effort produced great good. Our work continues because we are entirely committed to food safety and to ensuring human health.
Conquering Pathogenic Bacteria Is, In Fact, Quite Challenging
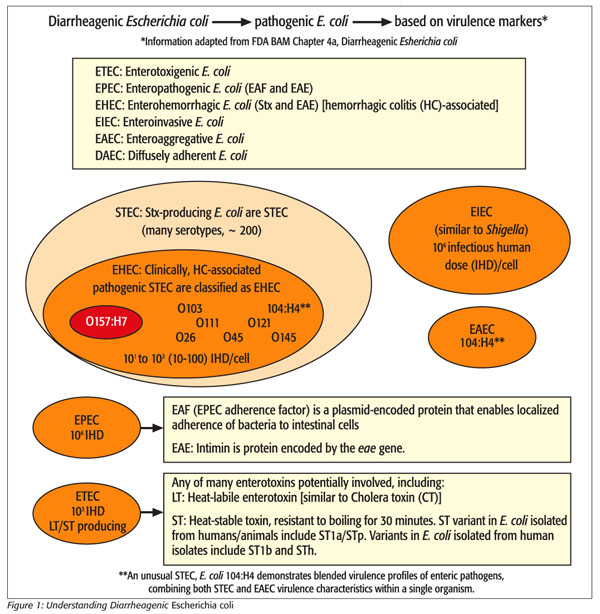 To understand the challenges of testing for pathogenic STEC, we need to understand E. coli diversity and the mechanics of what makes them deadly (see Figure 1). Combined virulence factors within pathogenic STEC are the building blocks that make this pathogenic STEC the deadly monster that it is. First is stx—the toxin-producing component. Second is eae (sometimes referred to as intimin)—the component that facilitates adhesion of the bacterium within the human digestive system. When these two virulence factors are present together within one E. coli bacterium, following ingestion, that E. coli attaches itself to the intestinal wall where it multiplies and undertakes the process of charging stx toxin into the host. Simply stated, a single E. coli having both stx + eae = pathogenic STEC.
To understand the challenges of testing for pathogenic STEC, we need to understand E. coli diversity and the mechanics of what makes them deadly (see Figure 1). Combined virulence factors within pathogenic STEC are the building blocks that make this pathogenic STEC the deadly monster that it is. First is stx—the toxin-producing component. Second is eae (sometimes referred to as intimin)—the component that facilitates adhesion of the bacterium within the human digestive system. When these two virulence factors are present together within one E. coli bacterium, following ingestion, that E. coli attaches itself to the intestinal wall where it multiplies and undertakes the process of charging stx toxin into the host. Simply stated, a single E. coli having both stx + eae = pathogenic STEC.
Today, we are faced with knowledge that in addition to E. coli O157:H7, other deadly foodborne pathogenic STEC can potentially make their way into our food supply, including the six soon to be regulated as adulterants: E. coli O26, O45, O103, O111, O121 and O145. We appreciate the value of validated and verified interventions currently working to reduce pathogens; however, we also understand that testing for E. coli O157:H7 does not determine the status of non-O157 STEC. Knowing this, our new challenge is similar to our experience in the 1990s with O157:H7—we must undertake the effort necessary to detect and control these additional six pathogenic STEC.
At this point, I want to be clear that the remainder of this article addresses only testing for non-O157 STEC. The reason for this distinction is that there are subtle differences between methods for O157:H7 testing compared with non-O157 STEC testing.
Developing STEC Testing Methods
Now that we understand the characteristics of pathogenic STEC, it’s important to differentiate between pathogenic STEC and other STEC. Surprisingly, stx-producing E. coli that do not have the eae component are not typically associated with severe illness. Classified as STEC, there are literally hundreds of stx-containing E. coli serotypes that actually will pass through the digestive system harmlessly, simply because they lack the adhesion factor—eae. It really is remarkable, but when the adherence factor eae is missing, the bacteria cannot attach to the intestinal wall and are removed from the body by natural processes. (One notable exception to this oversimplification, as punctuated by the summer 2011 sprouts outbreak in Germany and Europe, is E. coli 104:H4, which is characterized by stx combined with non-eae adherence mechanisms.)
One last point we should cover at this stage is the potential sources of eae that are not STEC. There are many types of eae and many potential bacterial sources of it. There are also several variants of stx. So our challenge of testing a sample to determine if it contains pathogenic STEC is complicated, because we now know that stx and eae could potentially come from two or more bacterial sources and the presence of both virulence factors alone in a composite sample is not necessarily cause for concern. A successful test must determine if both stx and eae are present and also that both originate from a single E. coli bacterial source, specifically E. coli O26, O45, O103, O111, O121 or O145.
Imagine the challenge for our scientists to develop a single test kit that will detect both eae and stx virulence factors in addition to determining the presence/absence of specific serotypes of E. coli that are known to be pathogenic STEC—E. coli O26, O45, O103, O111, O121 and O145. The challenge of numbers is compounded by the mechanical/physical limitations of the two most widely used and reliable rapid testing methods: polymerase chain reaction (PCR) and immunoassays. Quite simply, the number of factors to be tested exceeds the capacity of familiar PCR and immunoassay technology to provide results in a one-step test.
Several test kit manufacturers have been hard at work overcoming these challenges to provide the industry with reliable, easy-to-use, accurate test kits (see “Challenges for Non-O157 STEC Testing,”). We can expect in the months and years ahead that additional improvements will become available with the trend toward increasing the capacity to test larger numbers of genetic targets in a single test and sample-preparation enhancements that will increase speed and accuracy.
Today, test kit manufacturers have adopted a stepwise approach of detecting virulence factors stx and eae and sequentially testing presence/absence of O26, O45, O103, O111, O121 and O145. Flexibility in testing arrangements may allow for identifying O factors by either immunomagnetic separation or PCR and then virulence factors by PCR. Some kits offer the flexibility to test for O factor first and then to test for stx and eae virulence. Hopefully, your work of evaluating test kits and selecting the best method for your needs (see “Choosing a Non-O157 STEC Test,”) will be easier now that we have reviewed the details of how these kits work and the challenges of testing non-O157 STEC.
Jim Byron shares his extensive knowledge and diverse experience gained as an executive in the water, chemicals, food testing laboratory and test kits business. Byron was recruited to a leadership role in biotechnology and food safety in 2005. His scientific work in close association with food industry leaders, exposure to production systems and strong business foundation allow Byron to provide clear and useful information about Listeria testing to managers in today’s food production environment. He can be reached at 484.356.7283 or jb@xgenex.com.
Sidebar #1
Challenges for Non-O157 STEC Testing
Food Safety Magazine asked various companies within the food industry, What are the major challenges involved in non-O157 STEC testing? Several responses are provided below:
“Developing reagents that specifically detect the gene targets in the adulterated strains named by the U.S. Department of Agriculture, while at the same time minimizing cross-reactivity with detection of these same gene targets from nonpathogenic background or near neighbor organisms that can also be found in the beef sample. We accomplished this by integrating immunomagnetic separation prior to qPCR and using highly specific chemistry qPCR detection assays. Our workflow can help to minimize the potential for these false positives, while also providing the concentration and sensitivity needed for confident clearance of negative 375-g beef samples in as little as 8 hours.”
“The biggest concern right now is the development of a defined and industry-consistent process regarding the next steps companies should take if they get a STEC suspect on the available PCR screening methods.”
“Will the industry want to carry these through to cultural confirmation and if so, what is the expectation of industry regarding turnaround time and the effect this will have on product disposition?”
“The biggest challenge to developing tests for non-O157 STEC is insufficient understanding of all of the genetics relating to virulence factors. A single genetic marker that can separate virulent from avirulent strains has not yet been identified. Methods available today require a stepwise series of screenings looking for several genetic markers. All of these markers must be present. This screening approach adds a significant amount of time to the testing process and to getting a final test result.”
“A key challenge in testing for the ‘Top Six’ non-O157 STEC is the inability to easily and efficiently distinguish them from harmless bacteria using currently available diagnostic tools. This is based on the fact that nonpathogenic bacteria can naturally carry the same diagnostic markers associated with non-O157 STEC, yielding similar reactions that may implicate large amounts of products that are not contaminated with non-O157 STEC. Accordingly, additional analyses would be needed to determine if pathogenic bacteria are present, which at the time is limited to technically demanding, inefficient and expensive cultural confirmation techniques. The industry will benefit greatly from the much anticipated advances that can more efficiently and effectively differentiate non-O157 STEC from harmless bacteria that normally occur in agricultural products.”
Sidebar #2
Choosing a Non-O157 STEC Test
According to Tom Weschler, president of Strategic Consulting Inc. (www.strategic-consult.com), “2010 testing for E. coli O157 in the U.S. totaled 4.9 million tests, with red meat accounting for 80 percent or 3.9 million tests. In 2012, we project that STEC screening test volumes will eventually equal or exceed 2010 E. coli O157 test volumes, which represents a major shift in U.S. testing markets.”
Types of Tests: Today, our choices of STEC test kits include rapid methods based upon PCR detection or a combination of immunomagnetic separation with PCR. Soon, additional methods will be introduced to the market, increasing options available to the food safety professional. When selecting a test kit, it is important to understand how the method works and also how the method has been validated and certified. The following information is a review of test kit selection fundamentals.
Molecular methods are based on DNA detection by PCR. Following incubation of the sample in enrichment media, an aliquot is transferred for “amplification” of the target DNA using a thermocycler, which measures the change in concentration of DNA over time to determine the status of the sample—positive or negative. One method uses immunomagnetic separation to preferentially select E. coli having the target STEC “O” factors, which are then subjected to PCR analysis. Other methods perform multiple sequential PCR analyses to determine the status of the sample—positive or negative.
Validated & Certified Methods: Choosing a method that has been validated and certified by an appropriate independent authority increases your assurance that your investment in testing will withstand scientific scrutiny—and meet regulatory requirements. It is important to review the details of the methods you are considering to verify that the method has been validated for the food matrix you are testing and that you clearly understand other important factors such as sample size, media volume/ratio and enrichment time. You should use the online resources of the appropriate scientific authority in addition to requesting information from the test kit supplier. AOAC International is the primary U.S. authority for certifying test methods.
Inclusivity & Exclusivity: These data tell you what organisms the test will and will not detect. In addition to providing information about “true positives” that the test will detect, interpretation of the data helps you understand the potential for false-positive and false-negative results.
Inclusivity testing is performed by the kit manufacturer to determine from a broad range of organisms those that will produce a positive result by the test. In the case of STEC, a review of inclusivity data will indicate which E. coli are detected by the kit. If there are organisms that produce a false positive result, these may be indicated in the inclusivity data. By contrast, if there are target STEC that are not detected by the kit, then the absence of these will be your indication that the method may not detect all of the target STEC. It is important to review the inclusivity data when choosing a kit.
Exclusivity testing is performed by the kit manufacturer to test a broad range of non-target organisms that produce an accurate negative test result. These data provide additional information about the test accuracy—in this case, the ability of the test to accurately produce negative results for nontarget bacteria.
Sensitivity & Specificity: These measures capture the ultimate test accuracy compared with a reliable benchmark. Sensitivity and specificity are reported as a percent.
Sensitivity of 100 percent indicates that during the validation, there were zero false-negative results—in other words, all of the intended STEC were detected by the method.
Specificity of 100 percent indicates that during the validation, there were zero false-positive results—only target STEC intended to be detected were detected.
Sample Enrichment Media: Sample enrichment using nutritive media is necessary when testing food and environmental samples because of the very low prevalence of STEC and other pathogens in food products. Enrichment times vary based on the performance of the media in resuscitating weak or injured cells and the detection capabilities of the test assay. As you consider different test systems, you will have the opportunity to discuss enrichment media with your test supplier and evaluate the potential benefits of using conventional media or proprietary media. Here are highlights of each option:
Conventional Enrichment uses less expensive conventional media that may be acceptable when performance of the test assay is not affected. Cost savings are typically offset by the need for additional enrichment time.
Selective Enrichment for STEC takes advantage of optimization of the media to grow target STEC to the exclusion of other organisms. Additives included in the media formulation will prevent the growth of undesirable organisms while nourishing target STEC to grow faster in an environment where competition has been minimized. When deciding to use selective media, it is important to confirm that the media have been validated to work with your test assay.
Understanding STEC: A Growing Concern




